The incredible story of how the people of the Warsaw Ghetto beat typhus

In 1941, Nazi troops had forced 450,000 people from the city’s Jewish population into just a 3.4 square kilometre area. Image: REUTERS

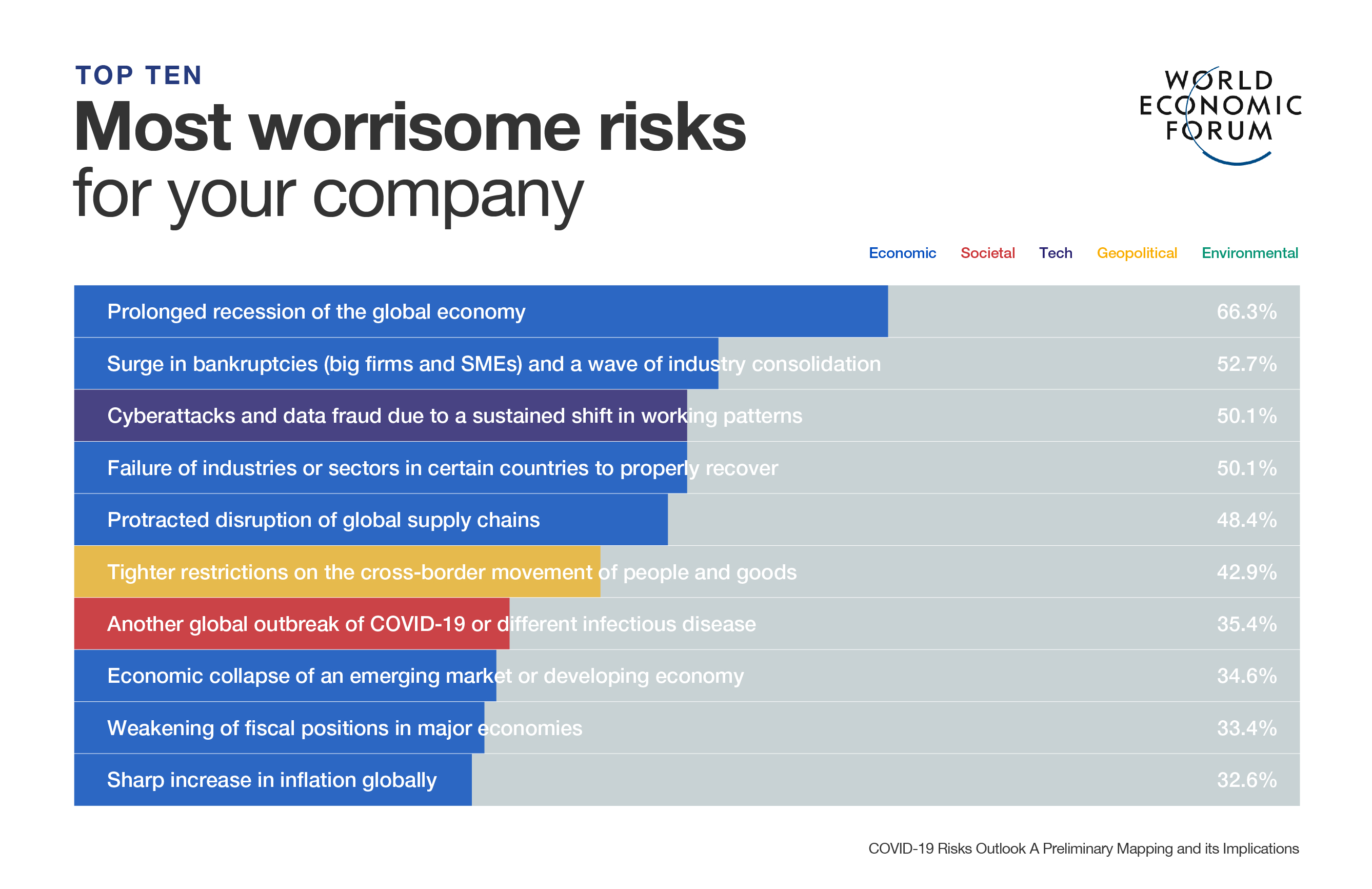
Explore and monitor how COVID-19 is affecting economies, industries and global issues

Get involved with our crowdsourced digital platform to deliver impact at scale
Stay up to date:
COVID-19
- In 1941, a typhus outbreak hit the Warsaw Ghetto, where 450,000 people were trapped by the Nazis.
- The cold, crowded environment provided the perfect conditions for infections to spread.
- But, as a new study finds, residents took measures to prevent infection – and wiped out the disease.
In January 1941, people in the Warsaw Ghetto started getting sick.
Nazi troops had forced the Polish city’s Jewish population into a 3.4 square kilometre area a few months earlier. As the new year began, fresh arrivals were brought into the sealed-off zone – and with them came typhus.
The 450,000 residents were suddenly facing an outbreak of an infectious disease that, without treatment, has a case-fatality rate of up to 40%. Conditions were ripe for the lice that spread the bacteria to proliferate. As well as poor hygiene, cold weather and starvation, inmates were dealing with a population density up to 10 times higher than any city today.
The disease tore through the ghetto. It infected as many as 120,000 people, and up to 30,000 died directly from typhus. Many more perished due to starvation, or from a combination of that and the illness.
Chillingly, it’s thought the Nazis knew this would happen. But what they hadn’t counted on was the inmates pulling together to beat the outbreak.

Remarkable response
By October that year, a harsh winter was approaching – and infections would have been expected to rise and rise. But instead the epidemic dropped off until it disappeared.
Why this happened is the focus of a new study published in the journal Science Advances. Using mathematical modelling and historical documents to investigate, the international team of researchers suggest public health interventions were responsible for eradicating the disease in the ghetto.
And they say their findings are directly relevant today.
The team’s modelling and statistical analysis estimates the epidemic was on course to grow two or three times larger. But – after scouring rare documents and publications from across the globe – they discovered a series of actions within the community could have changed the disease’s course.
Community efforts
Despite living in the bleakest of circumstances, the people of the Warsaw Ghetto rallied to help stop typhus spreading.
Residents were terrified of accidental contact and so practiced social distancing, the report says. People encouraged each other to be hygienic and keep their apartments clean. Self-isolation was also a regular occurrence.
And keeping people informed was a priority for the ghetto’s many experienced doctors and specialists. The study found evidence of training courses and lectures on public hygiene and infectious diseases – and even an underground medical university for young students.
“In the end, it appears that the prolonged determined efforts of the ghetto doctors and anti-epidemic efforts of community workers paid off,” says Professor Lewi Stone, the mathematician and disease modeller from RMIT University and Tel Aviv University who led the study.
“There is no other way we can find to explain the data.”
Essential cooperation
The Warsaw Ghetto’s story underlines the huge impact individual action can have on reducing the spread of a virus or bacteria, according to the authors of the study. Alongside government regulations, it’s the active recruitment of communities that beats epidemics and pandemics, they say.
There are other examples of this through history, including the experiences of places that “escaped” the 1918 flu pandemic. A US report focusing on seven remote locations across the country concluded that the communities “basically shut themselves down” to protect themselves.
Fast-forward to 2014, and during the Ebola outbreak in Liberia sessions organized across hundreds of towns and villages raised awareness of prevention measures and informed people how to care for the infected. The World Health Organization (WHO) declared the country free of the virus in early 2015.
What is the World Economic Forum doing to manage emerging risks from COVID-19?
And we’re seeing it today, too. New Zealand’s response to COVID-19 has been praised by the WHO. It credits clear communication for helping the public understand what was expected of them as key to the strategy that eliminated community transmission in the country. Polls show there was overwhelming support for the government’s approach.
Of course, even in the grip of a global pandemic, it’s hard to imagine the resolve it must have taken those in the Warsaw Ghetto to overcome the considerable obstacles in their way to beat typhus. The ultimate tragedy is that most of the people that survived the outbreak would soon after be taken to extermination camps.
But as Holocaust historian Stephan Lenstaedt, who helped assess the report’s modelling, says: “Unquestionably, there are invaluable lessons for us to learn from the past.”
Don't miss any update on this topic
Create a free account and access your personalized content collection with our latest publications and analyses.
License and Republishing
World Economic Forum articles may be republished in accordance with the Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International Public License, and in accordance with our Terms of Use.
The views expressed in this article are those of the author alone and not the World Economic Forum.
Related topics:
The Agenda Weekly
A weekly update of the most important issues driving the global agenda
You can unsubscribe at any time using the link in our emails. For more details, review our privacy policy.
More on COVID-19See all
Charlotte Edmond
January 8, 2024
Charlotte Edmond
October 11, 2023
Douglas Broom
August 8, 2023
Simon Nicholas Williams
May 9, 2023
Philip Clarke, Jack Pollard and Mara Violato
April 17, 2023