Chart of the day: How do the different COVID-19 vaccines work?

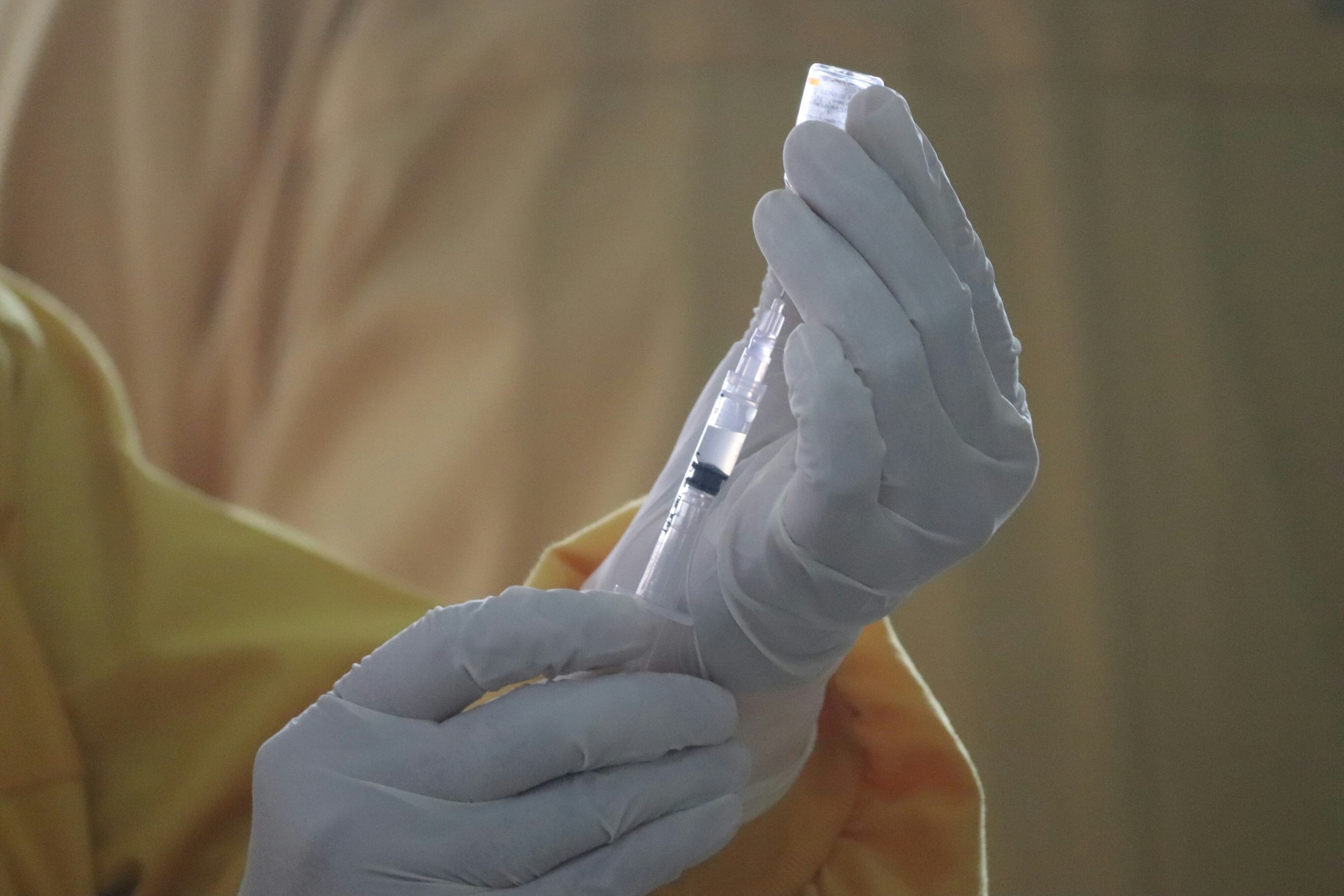
Vaccines against COVID-19 are starting to be rolled out around the world. Image: REUTERS/Amanda Perobelli

Get involved with our crowdsourced digital platform to deliver impact at scale
Stay up to date:
Vaccination
- Not all vaccines work the same way.
- This is how some of the COVID-19 vaccines work - and how they differ.
- Several vaccines are being used to tackle the pandemic worldwide.
The approval of the first COVID-19 vaccines has renewed hope across the world that the battle against the pandemic that has so far killed more than 1.6 million people may eventually be won.
No single vaccine is likely to be distributed globally; instead a range of treatments will be used. Here are two of the different vaccines and how they work.
The Pfizer-BioNTech vaccine
This RNA vaccine – one of the world's first to be approved – was developed by US pharmaceutical giant Pfizer and its German partner BioNTech. Its active ingredient is messenger RNA, which is closely related to DNA and contains a synthetic version of COVID-19’s genetic code.
Once injected, the patient’s immune cells follow the vaccine’s instructions to build the coronavirus ‘spike’ protein. Their body then launches an attack against it, thereby learning how to defeat the real virus. The vaccine, which requires two doses, has 95% efficacy rate. However, a significant drawback is that it needs to be stored at -70C.
The Pfizer-BioNTech vaccine received authorization for use by the UK regulator on 2 December. It has also been approved in other countries, including the US, Canada and in the European Union. US company Moderna has also developed an RNA vaccine, which has also been approved for use in the United States.
The Oxford-AstraZeneca vaccine
This viral vector vaccine was developed by the University of Oxford and AstraZeneca and works by altering a harmless adenovirus so it contains the genetic code for the coronavirus spike protein.
What is the World Economic Forum doing about access to vaccines?
The adenovirus is then injected into the body, where it transports the genetic instructions into the patient’s cells. These then start to produce the protein, triggering an immune response and priming the body to attack the real virus later.
The Oxford-AstraZeneca vaccine – which also requires two doses – has been approved for use in the United Kingdom. Research suggests that it could be up to 90% effective. It is both cheaper than its rivals and easier to store, meaning it could play a vital role in fighting the pandemic worldwide.
Don't miss any update on this topic
Create a free account and access your personalized content collection with our latest publications and analyses.
License and Republishing
World Economic Forum articles may be republished in accordance with the Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International Public License, and in accordance with our Terms of Use.
The views expressed in this article are those of the author alone and not the World Economic Forum.
The Agenda Weekly
A weekly update of the most important issues driving the global agenda
You can unsubscribe at any time using the link in our emails. For more details, review our privacy policy.
More on Health and Healthcare SystemsSee all
Shyam Bishen and Annika Green
April 22, 2024
Johnny Wood
April 17, 2024
Adrian Gore
April 15, 2024
Fatemeh Aminpour, Ilan Katz and Jennifer Skattebol
April 15, 2024
Carel du Marchie Sarvaas
April 11, 2024