The breathalyzer that transforms how we test for Covid-19

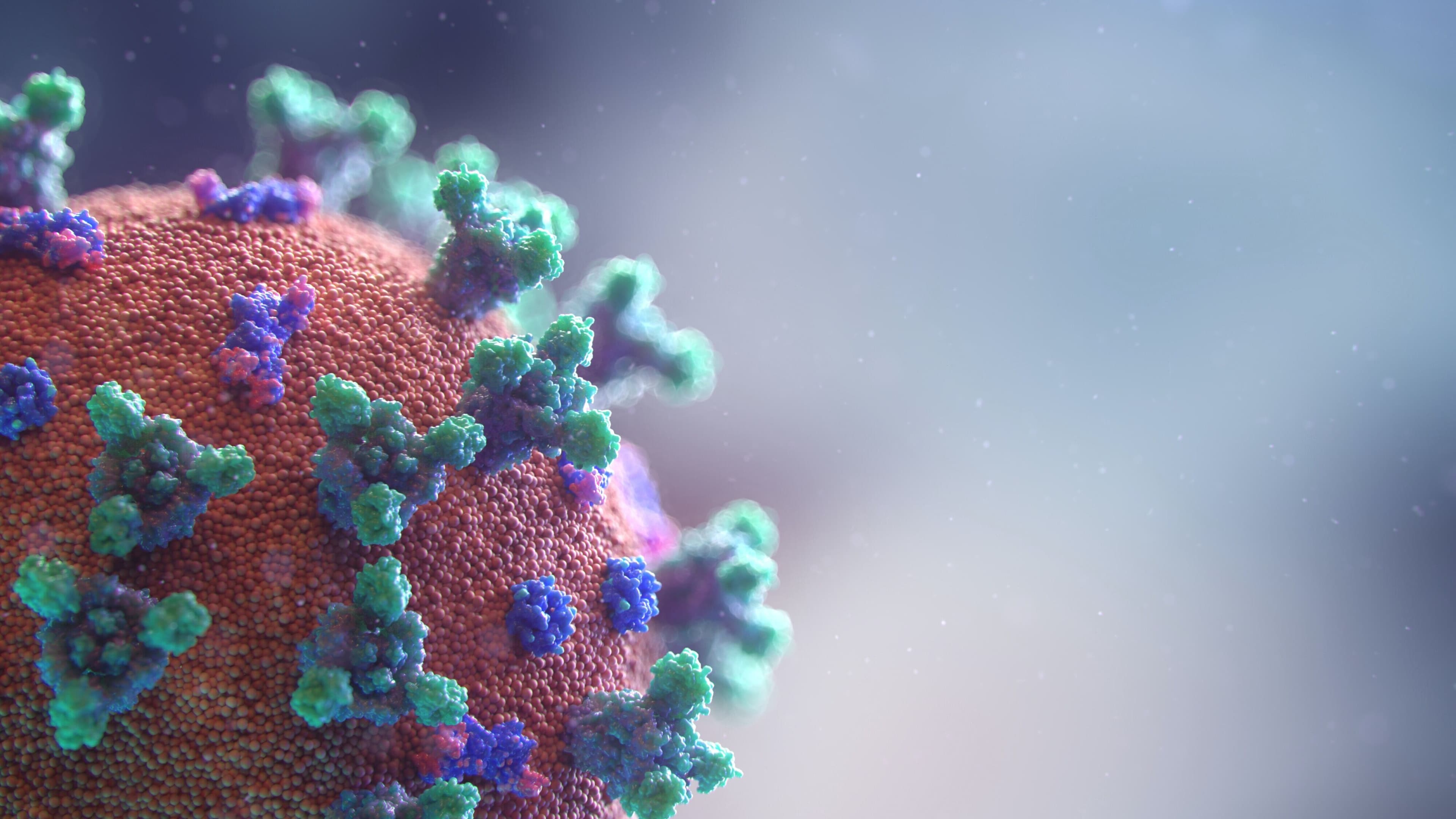
The device uses an enzymatic reaction mixture to detect viral RNA and convert it to DNA, where it can be measured using a PCR instrument. Image: Unsplash/National Cancer Institute

Explore and monitor how COVID-19 is affecting economies, industries and global issues

Get involved with our crowdsourced digital platform to deliver impact at scale
Stay up to date:
COVID-19
- Researchers have developed a unique method for detecting SARS-CoV-2 in breath samples using viral RNA detection.
- A study at Rhode Island Hospital determined that SARS-CoV-2 can be readily detected in the breath and is more predictive of lower respiratory tract involvement.
- Virus detection by the Bubbler is similar to a hospital-swab PCR test.
Researchers have developed a unique method for detecting SARS-CoV-2 in breath samples using viral RNA detection.
The researchers created a breathalyzer device they call “the Bubbler” that reverse-transcribes RNA from airborne virus particles into DNA, which can then be tested for COVID-19 via a common PCR test.
The device uses an enzymatic reaction mixture to detect viral RNA and convert it to DNA, where it can be measured using a PCR instrument. The Bubbler can also barcode that DNA, allowing a sample to be linked directly to the patient it came from and be used for sequencing.
In a new study in the Journal of Molecular Diagnostics, the investigators report on the design and testing of the device.
“The Bubbler is more likely to be a better indicator of current infection than nasopharyngeal swabs,” says lead investigator William G. Fairbrother, a professor in the molecular biology, cell biology and biochemistry department at Brown University.
The Bubbler is a glass tube with a glass pipette into which patients exhale. The tube is filled with a reverse transcription reaction mixture and cold mineral oil. The name of the device comes from the bubbling sound that occurs when the patient exhales into the device.
Breath beats mouth swabs?
For the study, researchers screened 70 patients treated in the emergency department at Rhode Island Hospital between May 2020 and January 2021 and tested samples from three points in the respiratory tract. They then compared saliva obtained from tongue scrapes in the mouth and samples of 15 seconds of exhaled breath collected in the Bubbler breathalyzer to a conventional nasopharyngeal swab PCR test.
The study determined that SARS-CoV-2 can be readily detected in the breath and is more predictive of lower respiratory tract involvement. Viral RNA is more enriched in the breath relative to oral samples, while oral samples include cells involved with SARS-CoV-2 replication that breath samples do not. This suggests the viral signal detected in the Bubbler comes from active viral particles, the authors say.
Tests for COVID-19 usually use samples collected from the upper respiratory tract by saliva or nasopharyngeal swab. Positive samples contain active virus, but viral load in the upper respiratory tract is not correlated with symptoms in the lower respiratory tract, such as pneumonia.
“Involvement of the lower respiratory tract is often a precursor to severe COVID-19, so there is an argument for a more direct sampling focused on exhaled breath,” Fairbrother says.
What is the World Economic Forum doing about access to vaccines?
Bubbler breathalyzer barcoding
Virus detection by the Bubbler is similar to a hospital-swab PCR test. However, because swab tests detect viral RNA fragments in cells that persist in previously infected cells, PCR tests can return a positive result for months after infection.
By contrast, the Bubbler detects airborne viral particles and is a better measure of risk of contagion, the authors say. It can also be adapted for environmental sampling in hospitals, transportation hubs, and closed environments like offices, ships, and planes, the investigators write in the study.
“Another advantage of the Bubbler is the barcoding, which enables high-throughput RNA virus testing at a fraction of the cost of conventional testing,” Fairbrother says.
The barcode returns a viral sequence that also supports strain identification, he says, which may prove useful as more information is learned about transmissibility and possible strain-specific treatment decisions. It can also be used for simultaneous batches of pooled samples, provides additional information such as viral load and strain identity, and eliminates the need for stabilizing a sample, potentially allowing the assay to be performed at home.
The investigators also demonstrated how the Bubbler might be adapted to detect virus in airborne samples. To model the movement of droplets exhaled in human breath, three unique nucleic acid samples were added to three personal humidifiers at different locations at varied distances from the Bubbler in a room with high airflow and a room with low airflow.
Although a detailed exploration of this application was beyond the scope of the study, the results demonstrate the potential to use aerosolized nucleic acids to quantitatively map airflow in indoor spaces, and to detect SARS-CoV-2 in the air.
“Such technology could be useful in restoring service to industries such as hotels, cruise ships, and casinos,” Fairbrother says. “There is also an epidemiological benefit to routine testing of air at early warning sites such as transportation hubs and hospital emergency departments.”
The National Institute of General Medical Sciences and the Roddy Foundation funded the work.
Don't miss any update on this topic
Create a free account and access your personalized content collection with our latest publications and analyses.
License and Republishing
World Economic Forum articles may be republished in accordance with the Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International Public License, and in accordance with our Terms of Use.
The views expressed in this article are those of the author alone and not the World Economic Forum.
Related topics:
The Agenda Weekly
A weekly update of the most important issues driving the global agenda
You can unsubscribe at any time using the link in our emails. For more details, review our privacy policy.
More on COVID-19See all
Charlotte Edmond
January 8, 2024
Charlotte Edmond
October 11, 2023
Douglas Broom
August 8, 2023
Simon Nicholas Williams
May 9, 2023
Philip Clarke, Jack Pollard and Mara Violato
April 17, 2023