Our health systems are under pressure. Here are 9 ways to remedy that

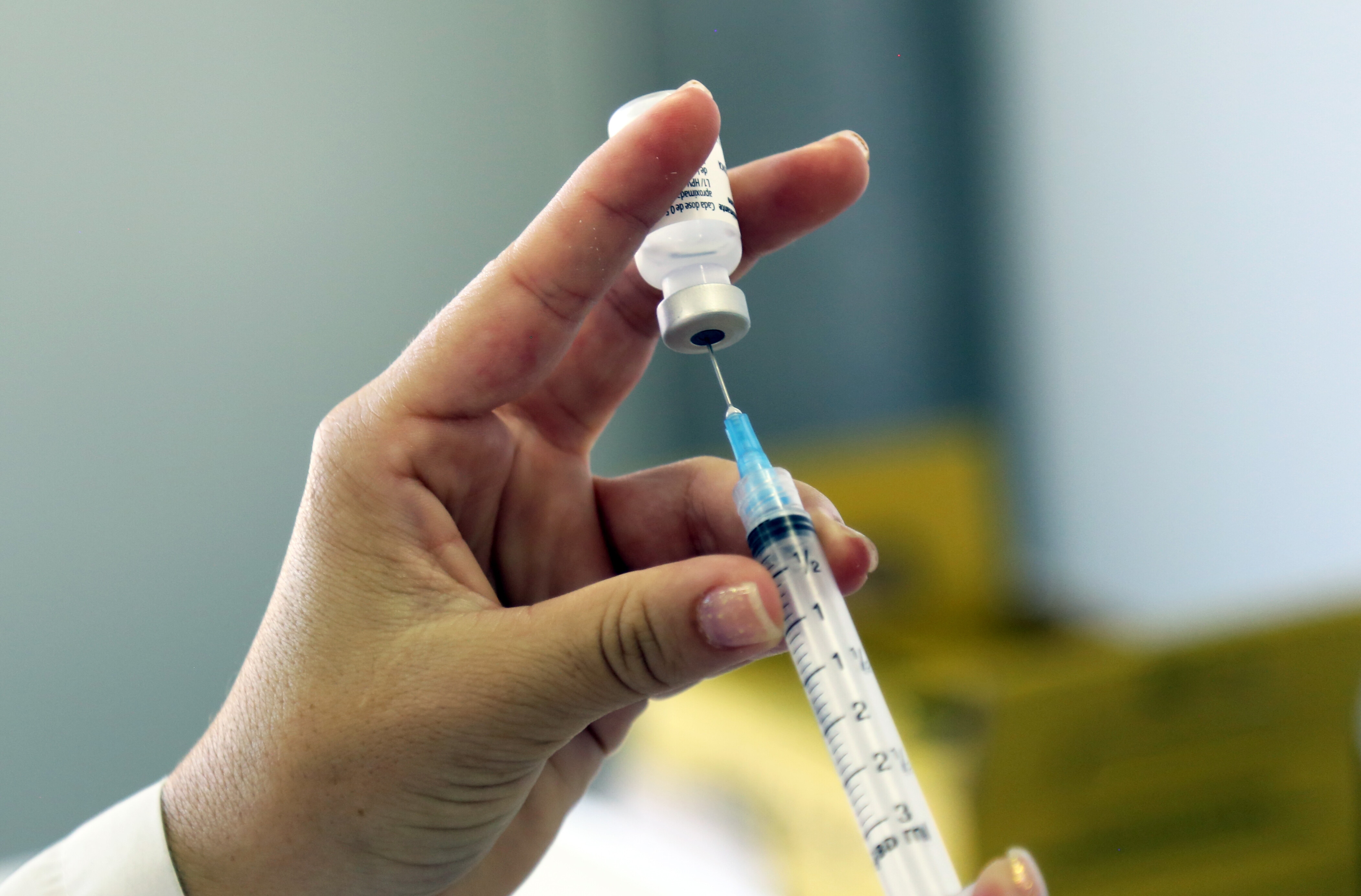
Technological advancement is nothing without the systemic changes needed to make healthcare fair for all. Image: Unsplash
The pressures facing health systems around the world are increasing, and they are diverse. Some populations are youthful and fast-growing – others are ageing. Fourth Industrial Revolution technologies are affecting the practice of medicine, and waste and inefficiencies are too often the norm. To overcome existing barriers to health and health service provision, and thereby to promote healthy lives and wellbeing for all by 2030, we must rethink, reorient and redesign the health systems of the future.
In a new report, A Vision for the Future: Transforming Health Systems, issued by the World Economic Forum’s Global Future Council on Health and Healthcare, we explore five potential scenarios for patient experiences around the world, showing what needs to change in the next decade to create well-functioning, resilient health systems that put people first.
It’s now possible for mobile technologies to support health promotion and access to services in all countries, including in low-income settings. Wearable technology, electronic health records and artificial intelligence can help people with diabetes and hypertension, including those who live in poor and/or remote locations, exchange information instantly with health professionals and para-professionals – but only if there is access to affordable devices and to health workers who can reach underserved individuals.
Improved genetic testing and diagnostics, along with precision medicine and digital pills, could help a breast cancer patient in a developed country detect cancer early, take preventive measures and undergo appropriate treatment – but only if there are incentives in the health system to support a patient’s entire health journey and maximise long-term outcomes.
Based on these findings, here are nine recommendations to guide policymakers:
Health policymakers alone can’t provide the best possible health outcomes for populations. The solutions to many of our health challenges will not be found in the health sector and do not lie only with government actors. The latter must work across sectors and silos to address current inefficiencies and inequalities in health systems.
The conditions in which people are born, grow, work, live and age affect their health – as shown, most recently, by the work of the World Health Organization’s Commission on Social Determinants of Health. National and international health agencies need to commit to meeting the needs of the poorest and to working at all levels to provide equal access and quality of health services.
Universal access to basic services which enables good health and ensures that people are not impoverished by illness, accident or disability is imperative. Decision-makers must ensure that budget allocations are focused on quality services and that resources are distributed efficiently, effectively and transparently.
Many illnesses could be avoided, or their progress slowed, by an increased focus on health promotion and disease prevention, and by countering pervasive pressures encouraging unhealthy lifestyles. For example, adequate nutrition and exercise can help reduce or control diabetes and heart disease, and good policy can discourage the dietary precursors of these conditions.
A strong primary health sector increases access to services and helps people stay healthy. For example, primary health care can provide immunization, antenatal care and chronic disease management, thereby reducing pressures on the hospital sector and encouraging a less hospital-centred approach for conditions that are not acute and/or life-threatening.
The healthcare systems of the future must empower and engage people and their communities in health services, supporting healthy lifestyle choices and being sensitive to local culture and customs. This requires increased access for underserved people and training for health workers who can reach them.
Technology solutions do not provide a quick fix; they need to be sustainable, accessible, locally relevant and designed to meet individuals’ needs. Achieving that will require a shift from the fragmented application of technologies towards platforms that can take advantage of the benefits of emerging technologies, like big data and analytics, for improving health services and access to them.
A question always to be asked about health spending is: does it deliver value for money? Optimizing “value-based care” requires governments to invest in essential services and health systems, and to optimize the impact of those decisions by ensuring there is a sustainable, skilled and motivated health workforce.
The lack of transparency and the current fragmentation of many existing health systems pose significant challenges. There is a clear need for improved policy and regulation, for measures of equity, efficiency and effectiveness that can monitor system performance, and for an emphasis on ethical standards and norms to ensure accountability and engage all stakeholders.
In summary, we require a societal and environmental transition towards healthier lifestyle choices, together with the re-engineering of health systems to monitor their performance and put people at their centre, alongside the provision of adequate funding which is allocated and spent according to clear priorities, and a culture of building partnerships to deliver good outcomes. That requires, inter alia, having support from lawmakers for the necessary legislation, and budget allocations at the national level, as well as engagement with communities and action across governments to ensure the design of health systems that leave no one behind.
Don't miss any update on this topic
Create a free account and access your personalized content collection with our latest publications and analyses.
License and Republishing
World Economic Forum articles may be republished in accordance with the Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International Public License, and in accordance with our Terms of Use.
The views expressed in this article are those of the author alone and not the World Economic Forum.
Stay up to date:
Healthcare Delivery
Forum Stories newsletter
Bringing you weekly curated insights and analysis on the global issues that matter.
More on Health and Healthcare SystemsSee all
Andrea Willige
May 1, 2026