3 tactics to overcome COVID-19 vaccine hesitancy

Efforts to convince skeptics to get a COVID-19 vaccination should focus on thoughts and feelings about vaccines. Image: Unsplash / @diana_pole
- Public health officials could use advertising theory to achieve herd immunity to COVID-19, marketing experts believe.
- Efforts to encourage vaccinations to date have focussed on distribution but addressing how people think and feel about getting the vaccine could convince skeptics to vaccinate.
- Community leaders and local health workers can play a key role in tackling vaccine-related fear and misinformation, while incentives from states, cities and employers could help get skeptics through the door of local vaccination centres.
An estimated 60-70% of the world’s population needs to be vaccinated against COVID-19 to achieve herd immunity. This makes overcoming COVID-19 vaccine hesitancy, procrastination, and rejection the greatest marketing communication challenge of our lifetime.
The US is moving “from a supply problem to a demand problem,” as Dr David Kessler, the chief science officer for the US government’s COVID-19 response task force noted earlier this year. Research indicates that other countries including Australia, France, Russia, South Africa, Japan and Germany will face similar demand problems once their vaccine production and distribution issues are addressed.
There are simply not enough patient-centric solutions to address vaccine hesitancy, procrastination, and rejection. Our research focuses on creating and implementing such solutions to inform, persuade, and convince customer segments to act, and we believe this kind of approach could also boost COVID-19 vaccine communication efforts.
Patient-centric solutions to vaccine hesitancy
The decision-making process for customers - or in this case patients - is often understood using the Hierarchy of Effects Framework. It suggests that customers think first, then feel and then do. In relation to the COVID-19 vaccine, this implies that patients need to first “think” about it, that is, become aware of and knowledgeable about the vaccine. Next, patients need to “feel” positively about it, as in developing a conviction to get the vaccine. Finally, patients need to “do” it - in other words, get vaccinated.
Most policy makers have emphasised the “do” stage by focusing on distribution and convenience via a combination of mass vaccination, hospital, physician, and drug store sites. This makes sense for the population interested in getting vaccinated. For the vaccine procrastinator, hesitant, and rejector populations, however, we need to focus on the “think” and “feel” stages of decision making. Without these stages, patients are unlikely to move to the “do” stage.
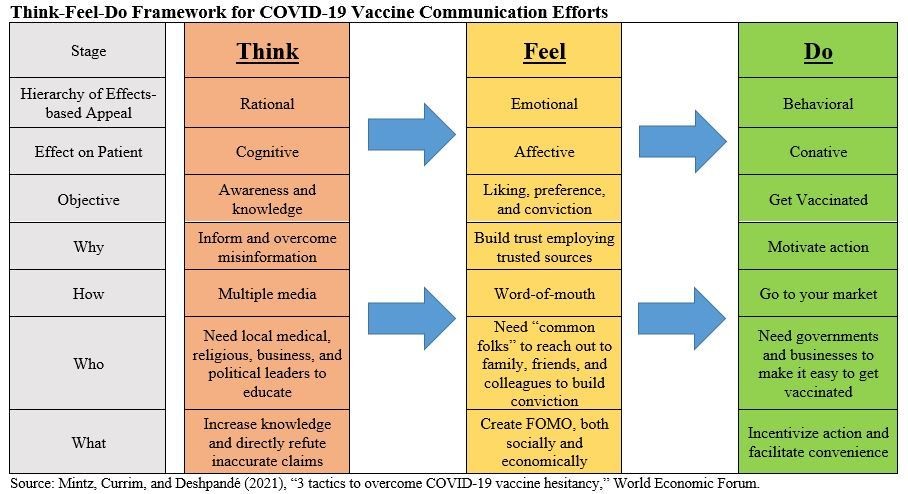
Using examples from the US - one country currently facing a greater vaccine demand than supply problem - we have developed three recommendations for how best to use this theory to eradicate vaccine hesitancy.
1. Increase knowledge and overcome misinformation
First, we need to focus on the “think” stage by asking why people are hesitating, procrastinating, and rejecting the vaccine. Research shows a major reason is that such patients are likely to believe the invention and approval process of the vaccine was rushed, with underreported side-effects. This can be addressed by local leaders proactively reaching out and educating sceptics via media such as phone calls, direct mail, television, billboard, and digital channels.
One rural parish in the US state of Louisiana, for example, enlisted African-American preachers and local leaders to directly phone members of their community. This led to a 9% increase in the parish’s vaccination rate in a week.
The state of Iowa features a current congresswoman who is also an experienced physician in its vaccine ads. This approach often appeals to preferences to hear from leaders in their own political party with medical expertise, while empowering them to make personal decisions without pressure.
Overcoming COVID-19 vaccine hesitancy, procrastination and rejection is the greatest marketing communication challenge of our lifetime.
”More assertive approaches are also needed to overcome vaccine misinformation, in particular on social media. Previous research shows that having medical sources directly refute inaccurate claims online is particularly effective. Training and funding is needed to help medical, public health, and non-profit organisations actively respond to misinformation with science-based evidence.
2. Improve feelings
The vaccine-hesitant population has developed strong feelings against it, so using information sources trusted by these people could improve their feelings about the vaccine. Research indicates those that are hesitant trust medical providers, political and faith-based leaders to provide “think”-based knowledge about medical decisions, but are more likely to rely on their communities to provide the “feel” or emotion-based conviction for decisions.
One nurse in Louisiana deployed a particularly effective tactic. She called her vaccine-hesitant patients to talk about how she had been a vaccine skeptic but changed her mind after her husband passed away due to COVID-19.
In the US state of Oregon, Native American tribes have seen relatively high vaccination rates. Among initiatives rolled out by these communities to encourage vaccinations, the Confederated Tribes of Siletz Indians has used direct phone calls, discussions, and social media apps to get family and friends vaccinated.
Another way to improve vaccine sceptics’ feelings is to play into a fear of missing out (FOMO), both socially and economically.
3. Facilitate action
Mass vaccination sites are critical to facilitate patients who want to be vaccinated. Reaching people that are unsure about getting vaccinated, however, will require proactive tactics.
First, incentives can work. Several US states and cities provide cash incentives and free transportation, or create lotteries and large block parties to incentivise vaccinations. Businesses should also be encouraged to contribute by providing paid time-off, free products and lottery giveaways.
Enhancing the convenience of getting vaccinated is another useful tactic. In business, we call this “going to your market” or, in this case, “taking the vaccine to the patients”. For example, the Primary Health Network in Pennsylvania, US created a mobile health unit to provide pop-up clinics in rural and underserved areas with larger vaccine-hesitant populations. The Southwest Health System in Colorado created “vaccine swat teams” to reach long-term care facilities and homebound residents who experienced difficulty getting to mass vaccination sites. Such approaches provide proactive micro-vaccination sites tailored for the vaccine-hesitant, procrastinators, and rejectors, in contrast to mass vaccination sites for those eager to get vaccinated.
We believe applying the “think - feel - do” patient-centered approach to the COVID-19 vaccine communication problem will improve efforts at accelerating global herd immunity. Ensuring a safe economic reopening and recovery and overcoming this significant health and economic challenge could depend on such tactics.
Don't miss any update on this topic
Create a free account and access your personalized content collection with our latest publications and analyses.
License and Republishing
World Economic Forum articles may be republished in accordance with the Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International Public License, and in accordance with our Terms of Use.
The views expressed in this article are those of the author alone and not the World Economic Forum.
Stay up to date:
COVID-19
Forum Stories newsletter
Bringing you weekly curated insights and analysis on the global issues that matter.
More on Health and Healthcare SystemsSee all
Mansoor Al Mansoori and Noura Al Ghaithi
November 14, 2025







