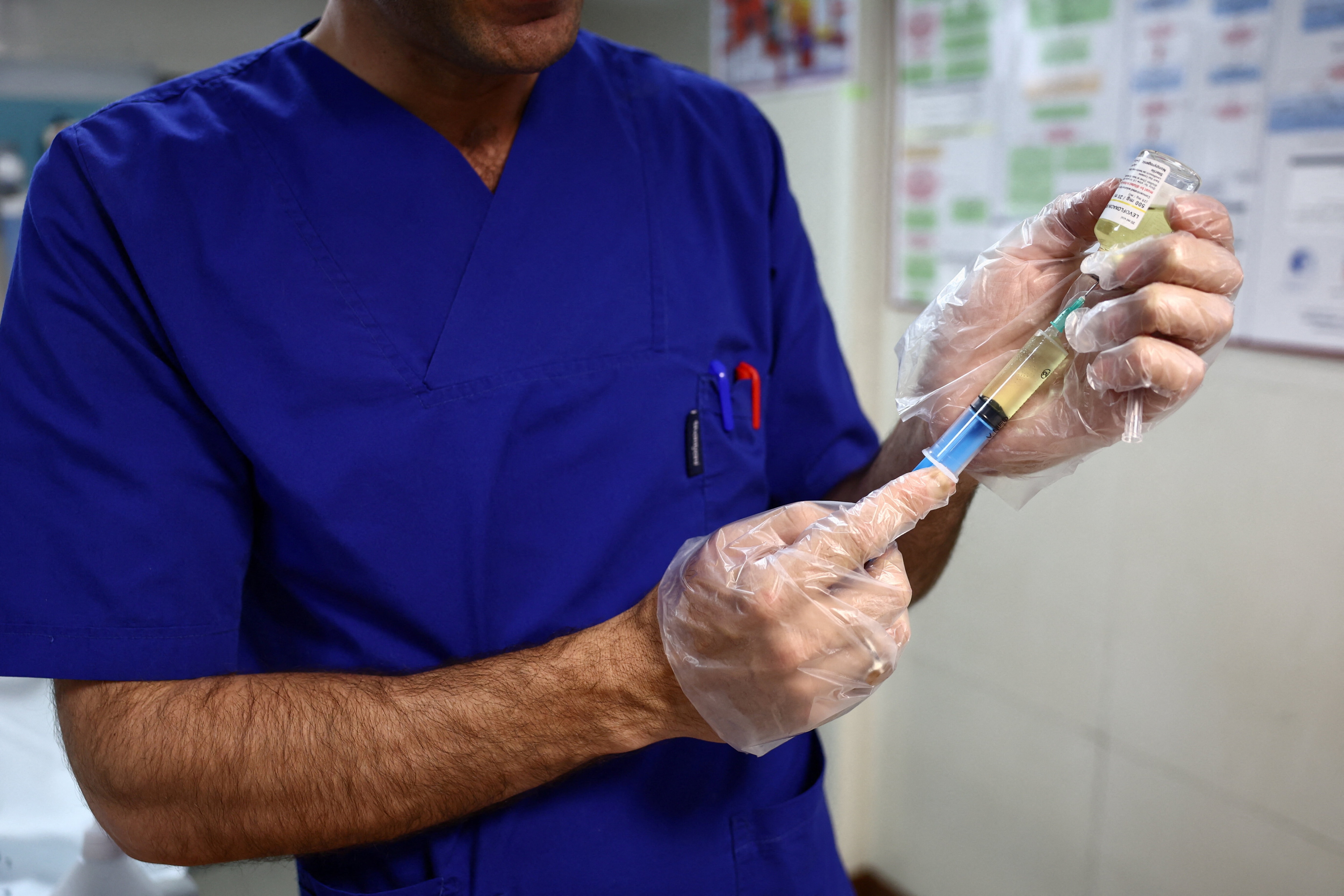
Are we acting fast enough on antimicrobial resistance?

Antimicrobial resistance affects all countries, although Africa is likely to bear the heaviest burden. Image: Pexels/Pixabay
Shyam Bishen
Head, Centre for Health and Healthcare; Member of the Executive Committee, World Economic ForumListen to the article
This article has been updated.
- As World AMR Awareness Week begins, experts warn that antimicrobial resistance (AMR) could lead to 10 million deaths annually by 2050 if left unchecked.
- Global initiatives like the Davos Compact, alongside advocates such as the UK's Dame Sally Davies, are helping to drive a "One Health" approach to protect essential medicines.
- In the fight against resistance, a new antimalarial drug promises over 97% effectiveness in recent trials.
In 1928, Alexander Fleming discovered the first antibiotic, penicillin, and by the 1930s, the first antibiotics had become commercially available.
Now, less than a century later, we are facing a health crisis as many drugs that have commonly been used are no longer effective and we struggle to find new treatments to combat infections.
This struggle is the focus of World AMR Awareness Week, running from 18-24 November. The 2025 theme, 'Act Now: Protect Our Present, Secure Our Future' demands immediate global investment to stop the slide towards a post-antibiotic era.
So-called 'superbugs', which have become resistant to the medicines once used to treat them, kill an estimated 5 million people a year. This antimicrobial resistance (AMR) has been described as “one of the biggest threats to global health, food security and development today”.
"Antibiotics underpin modern medicine," says the UK government's special envoy on antimicrobial resistance, Dame Sally Davies.
"I can't conceive of cancer care effectively without antibiotics, let alone many operations, including caesarean sections, transplants, or diabetic care. All of these need antibiotics because people are prone to life-threatening infections."
Davies has been advocating for a united approach to tackling AMR for over a decade, including making systemic changes and rethinking how we use antibiotics in humans and animals, as well as supporting and incentivizing the discovery of new drugs.
Without urgent action, she says, we risk a return to the pre-penicillin time when common infections were life-threatening, setting back decades of medical progress.
What is antimicrobial resistance?
AMR occurs when microbes – bacteria, fungi, parasites and viruses – evolve to the point where antimicrobial drugs that previously worked against them are no longer effective. As a result of this drug resistance, infections spread and become harder to treat.
Some strains of bacteria have become “superbugs”, developing resistance to multiple forms of treatment. These include MRSA (methicillin-resistant Staphylococcus aureus), Clostridium difficile (C. diff) and the bacteria that cause multi-drug-resistant tuberculosis.
AMR affects all countries, although some are feeling the impact more than others. In particular, Sub-Saharan Africa may bear a particularly heavy burden. However, there is currently a lack of high-quality data on AMR and infectious diseases in low-income areas, researchers say.
We urgently need more innovative, high-quality antimicrobials as resistance spreads and drugs such as antibiotics become less effective.
Why is AMR such a problem?
AMR directly caused 1.27 million deaths globally in 2019 and contributed to an additional 4.95 million deaths. This makes it a bigger killer than HIV/AIDS or malaria. Forecasts suggest that by 2050 AMR-related deaths will be 70% higher than they were in 2022. Improving access to healthcare and effective antibiotics could save 92 million lives between 2025 and 2050.
The impacts aren’t limited to health alone. The global economy will also be affected by higher healthcare costs, reduced productivity and an increase in poverty as a result of antimicrobial resistance. Without action, it could reduce global GDP by $3.4 trillion and drive an additional 24 million people into extreme poverty, the United Nations (UN) warns.
How does resistance arise?
Natural variations in the genetic makeup of microbes cause resistance to develop over time as they reproduce. For example, alterations in their DNA could mean antimicrobials can no longer reach the microbe cell or make microbes capable of creating enzymes that destroy the antimicrobial. Through natural selection, these microbes with advantageous traits will proliferate over less-resistant strains, spreading the genetic advantage more widely.
Microbes, like bacteria, are also able to directly transfer genetic material to each other in various ways other than reproduction.
Although both of these ways of transferring genetic material occur naturally, poor use of antimicrobials, among other things, can speed up resistance development and spread. For example, if an antibiotic course does not completely kill off an infection, we leave behind the microbes best able to fight against the drug. These will then multiply and pass on their survival traits.
How does antibiotic use affect resistance?
Excessive antibiotic use is a significant driver of resistance. If the treatment is too short, weak, or incorrect for the infection, we risk leaving behind resistant microbes. The more we expose microbes to antimicrobials and/or other resistant microbes, the more opportunities we create for resistance to develop and multiply.
And it’s not just prescribing to humans that is a problem – two-thirds of antibiotics globally are used in farming. In recent years, antibiotic use in agriculture in Europe has fallen dramatically. But they continue to be widely used in emerging economies because of their impact on profit margins and a lack of viable and affordable alternatives.
"We've got to use the treatments, the antibiotics, the antivirals, antifungals carefully, only use them when we need them," Davies explains, "but we also need to use them carefully in animals. If the animals are sick, of course they need treating. But actually, if it's just because it's cheaper than infection prevention and control then that is not acceptable."
How the Forum helps leaders strengthen health systems through collaboration
The role of the environment and climate change
The environment and climate change also have a role to play in the emergence, transmission and spread of antimicrobial resistance, as a recent report from the UN points out. Pollution from healthcare, pharmaceuticals, food and agriculture – such as wastewater from hospitals or agricultural runoff – is particularly problematic, as it may contain both antimicrobials and resistant organisms.
Introducing these to the broader environment will also impact biodiversity and soil health.
Indeed, research published in The Lancet points to a link between AMR and air pollution. Researchers studied the possible impact of air pollution (PM2.5) on antibiotic resistance in 166 countries, and those with higher levels of air pollution were also found to have higher levels of AMR.
Poor sanitation and access to clean water is another major contributory factor. In countries that lack these basic hygiene measures, water is the primary vector by which antimicrobial resistance and its associated diseases are spread. Improved sanitation, water treatment and basic hand-washing and hygiene facilities are crucial steps in curbing the spread of AMR, as the World Economic Forum points out in a briefing paper.

How can we turn the tide on AMR?
Global coordination is needed to tackle the rise of antimicrobial resistance as well as foster the development of new drugs.
Innovation is already proving vital. Novartis and the Medicines for Malaria Venture announced a new antimalarial drug, GanLum, on 12 November. In trials across 12 African countries, it was more than 97% effective against malaria, even in regions where resistance to current treatments is rising. Experts have likened the drug to a "fire extinguisher ready for the coming blaze" of resistance.
We must also work together to ensure healthcare systems worldwide are prepared for rising resistance and infection levels. This involves taking a 'one health' approach to combat AMR, which recognizes the connection between people, animals, plants and the environment they share.
For example, during the World Economic Forum's 2025 annual meeting in Davos the Forum’s Global Future Council on Tackling Antimicrobial Resistance developed and released the Davos Compact on AMR.
This compact outlines how the public and private sectors can engage and highlights the key areas of focus to tackle AMR. This will inform the work of the Unified Coalition for the AMR Response (UCARE), a collaboration between governments, philanthropic organizations and the private sector, which was launched by the Forum’s Centre for Health & Healthcare in Davos in January 2025.
UCARE is focused on:
- Supporting innovation and improving access to new and existing antimicrobials, diagnostics and vaccines;
- Building awareness and advocacy of AMR among policymakers and the public;
- Creating sustainable food and agricultural systems; and
- Promoting multi-sectoral engagement and funding.
Given the length of time it could take to develop new treatments, Davies echoes the need to focus on these areas.
"I'm calling on leaders to fund the research, to find new treatments and new vaccines and prevention," she says.
"Studies show the payback is massive, that it pays off over 10 to 30 years, 10 times. So make that investment, save lives, save your economies, save the food chain."
Don't miss any update on this topic
Create a free account and access your personalized content collection with our latest publications and analyses.
License and Republishing
World Economic Forum articles may be republished in accordance with the Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International Public License, and in accordance with our Terms of Use.
The views expressed in this article are those of the author alone and not the World Economic Forum.
Stay up to date:
Global Health
Forum Stories newsletter
Bringing you weekly curated insights and analysis on the global issues that matter.
More on Health and Healthcare SystemsSee all
Manica Balasegaram
May 22, 2026