The world's health sector is expanding. Can it heal our economies?

Economic engine ... the health sector is expected to create tens of millions of new jobs Image: REUTERS/Daniel LeClair
All over the world, the health sector is predicted to be the largest source of job creation for the next decade.
Its growth is being driven by increasing numbers of older people and by the expansion of the global middle class. As these two groups grow, the higher levels of healthcare they demand will cause seismic shifts in the amount of money being spent in the health sector, driving employment.
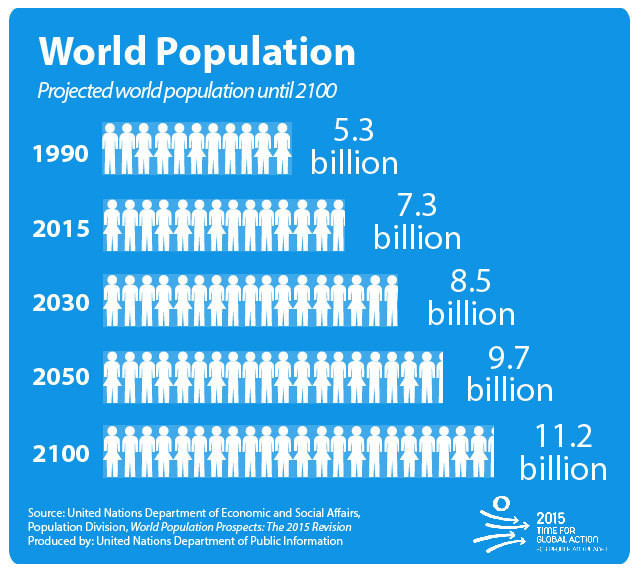
Even without these trends, the world would need millions more health workers. But even though more health workers are being trained than ever before, population growth is currently outstripping increases in training.
The world no longer dominated by infectious diseases requiring episodic treatment, and is instead becoming dominated by non-communicable, chronic diseases such as heart disease, diabetes, cancer, and mental-health conditions, which require continuous treatment.
Unlike traditional employment sectors such as agriculture and manufacturing, which shed jobs as technology advances, healthcare tends to add jobs with increasing technology. The health sector will be an economic engine that not only creates new jobs and business but, by making workers in other sectors healthier and more productive, will enable those sectors to grow faster. Tens of millions of new jobs will be created.
But what to do about it?
How do we ensure that the rising number of health-sector jobs avoids wasting money and instead results in improved healthcare at low cost that connects with other sectors and produces the sort of jobs that people can thrive and advance in? Partly in an effort to answer these questions, United Nations Secretary-General Ban Ki-moon has launched the Commission for Health Employment and Economic Growth.
So how can we make sure the greatest good comes out of investing in these additional health jobs? There are several actions that could help:
1. Fix the broken educational system
Currently, the health-sector educational system is one of the most expensive and fragmented anywhere. Theory often receives more time than competency-based education, and significant new educational requirements are frequently added by disconnected regulators with little or no evidence that the changes will improve the health of the majority of patients. Many countries have driven up the cost of health-worker education to the point of pricing themselves out of health-worker self-sufficiency. Most schools are run as boutiques and don’t make use of digital learning or the latest wisdom in adult learning. We need global public goods such as open-copyright curriculae for the world’s most recognized professions – nursing, midwifery, medicine, and pharmacy. Governments must coordinate regulators, reduce barriers to the establishment of private schools, and create pipeline programmes for students from minority and under-served communities.
2. Create career paths:
Demotivated and absent health workers plague most health systems in emerging economies. Offering decent career paths could motivate the rapidly increasing number of health workers and ensure better performances. In such systems, a high-performing health worker knows that he or she will be able to advance either technically or managerially. The creation of career paths will be especially helpful in engaging young people in the health-sector job markets. Career paths create entry-level jobs that help young people and those from poor backgrounds on to the first rung of the career ladder. The current lack of career progression can exclude younger generations and the poor from these promising jobs. For example, an analysis by IntraHealth revealed that less than 4% of health workers in Senegal are aged 19-30, despite that age group constituting around one-quarter of the population.
3. Address gender challenges
If the growth of health-sector jobs is to improve equity, we must address the gender challenges in health-sector employment. Women tend to be segregated in the lowest-paying jobs in healthcare; whichever profession they are in, they tend to advance more slowly than their male counterparts. Countries must rebalance wages and benefits to truly reflect the skills and risks involved in each job. They must also support women to enter the health profession of their choice, and ensure that women have what they need to succeed and advance in their chosen healthcare profession.
4. Modernize management
Better management can be achieved through the training and hiring of professional managers and adding management competencies to the training of clinical health workers. Other efficiencies will come through the introduction of digital health tools such as smartphone electronic medical records, which will increase judicious use of data, help individual health workers become more efficient and more accountable to health systems and communities.
5. Rationalize financing
Greater investment is needed in health workers throughout the span of their careers, from education to retirement. This rationalized financing includes: access to student loans and scholarships; targeted financing for students at risk of dropping out of school (as high as 60% in many countries); access to loans to start private practices (which add to the resilience and diversity of the health sector); payment systems that incentivize health workers to act in a way that improves the health of their patients and communities; and retention packages to increase the numbers of health workers serving the neediest communities.
Additional thorny issues will arise. There are still disagreements over the role of immigration in the global health labour market, for instance. Also, some argue that those countries with the most cost-effective training should train the rest of the world’s health-workers, while others object to the importing of health workers, arguing that it results in under-investment in educating young people in the receiving countries.
Telemedicine, too, will raise serious questions about trade in services, accountability and the cultural components of health. As will the rapid growth and consolidation of the private health sector in developing countries, which will pose interesting advantages and challenges.
But no matter what happens, it is clear that any country that plans and acts for the growth in the labour markets of its health sector will be a country that comes out ahead – both in terms of the health of its population and the health of its economy.
Have you read?
What can technology do for global health?
These countries are getting healthcare spending right
How do we make healthcare fit for the future?
The 69th World Health Assembly takes place in Geneva from 23-28 May 2016.
Don't miss any update on this topic
Create a free account and access your personalized content collection with our latest publications and analyses.
License and Republishing
World Economic Forum articles may be republished in accordance with the Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International Public License, and in accordance with our Terms of Use.
The views expressed in this article are those of the author alone and not the World Economic Forum.
Stay up to date:
Future of Global Health and Healthcare
Forum Stories newsletter
Bringing you weekly curated insights and analysis on the global issues that matter.