The ageing population is a threat to women’s economic welfare

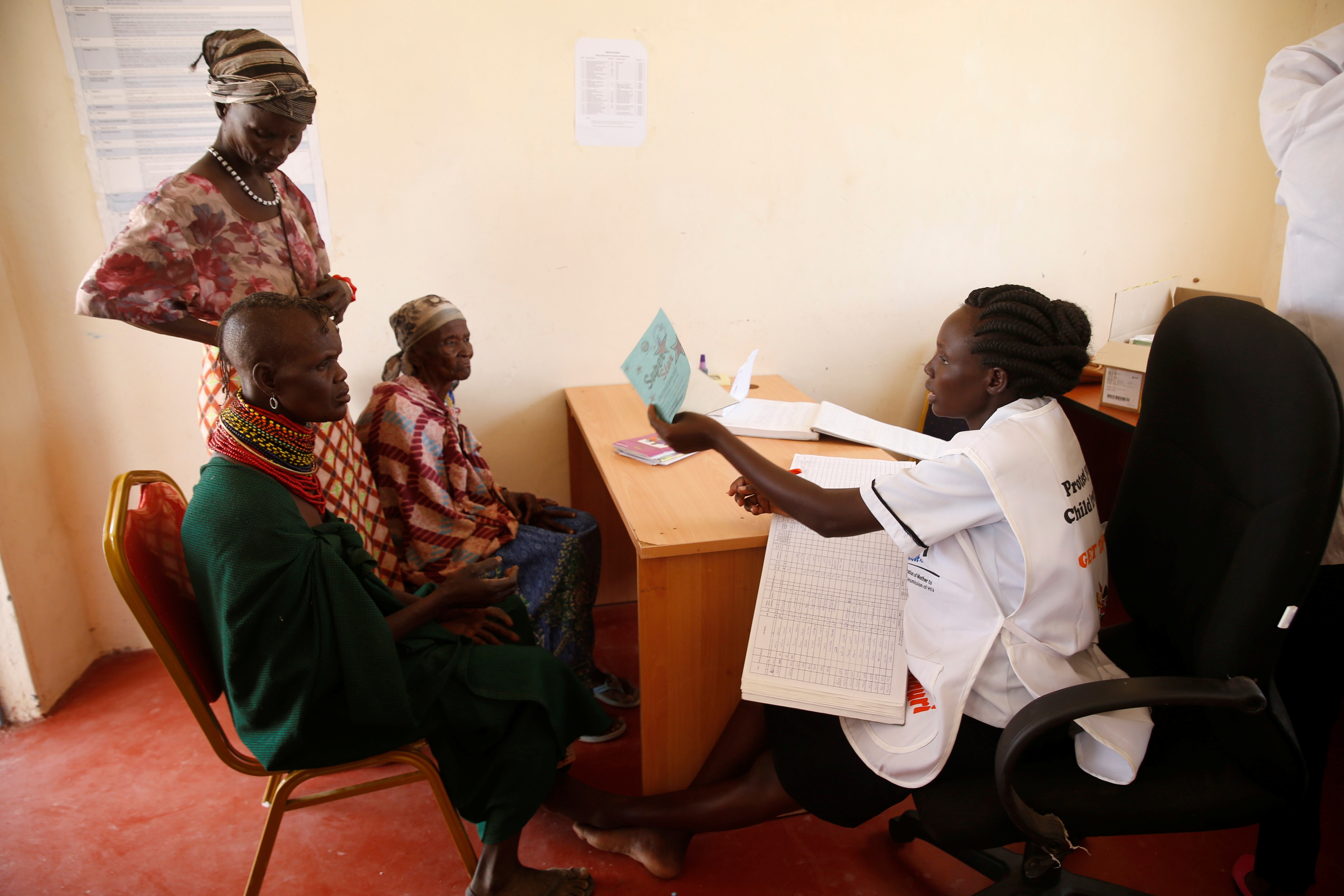
The ageing population population poses a financial risk to women. Image: REUTERS/Thomas Peter
Many women in the UK are unaware of the financial risk they face. A financial risk brought about by the ageing population.
Across the globe, about two thirds of informal care for frail older people falls to female relatives. Men are also carers, but women do this work more often, both in developed and developing countries, in every culture. Even where a woman has work outside the home, she is more likely than a man to become the direct carer for the frail older people in their family.

Disproportionate burden
In patriarchal societies, caring work is of lower status than work outside the home and is allocated to women. In cultures with established social and legal gender equality, it still makes economic sense in any family for a lower paid person, which is more usually a female, to give up work to do any unpaid caring. In addition, there are cultural norms that allow women to do personal care for both males and females, where it would be unacceptable for a man to do intimate care for a woman.
Men who are carers also face a major carer burden, but more often they start off better financially equipped to buy their way out of the problem. Women, on the other hand, are more likely to have been part-time workers, to have taken maternity career breaks, or to have worked in low-waged sectors such as health and social care, if they have been employed at all. Caring work drains people of time, money and opportunities.
When women leave the home to enter the workplace, some of their housework becomes institutionalised and professionalised. The creation of nurseries for childcare has allowed mothers to continue to earn and develop a career while children receive early developmental support from paid workers. A child is a major expense, even though child rearing is supported by maternity and paternity pay, free nurseries and years of free child minding through state schools. Without state support, having children would be unaffordable for some. Even with support, mothers who want or need to work know they have to plan families carefully.

Cared for by the state
In the UK the creation of geriatric hospitals took the continued care of frail older people away from women at home when the National Health Service began in 1948. From that moment, people in the UK began to believe that aged care would be provided by the state free at the point of delivery. At first, they were right.
But since then, local and national government support for aged care has diminished, particularly over the last 30 years. In 1979, a new Conservative government inadvertently created perverse incentives for people to enter care and there was an explosion of private residential homes in which residents were funded by the state.
That state policy on subsidising residential care was reversed by the 1990 NHS and Community Care Act. This was because the cost of care and the demand was already increasing exponentially as the population aged. In recent months, living wage regulations caused another stepped increase in the cost.
Not likely to improve
There is every reason to believe that this trend of reduced state aid against a background of increased prices will continue. In south-east England, nursing homes were charging, on average, £851 a week even before the living wage increase for care staff. And still there is a residual misconception that the state will pay for it. Long-term care insurance to cover this is almost impossible to buy in the UK.
Unless there is a major UK policy and resources shift, women need to plan for a future where their career and personal finances will be significantly affected by caring for older relatives. Employers, local authorities, insurers, health services and culture may change, but it would be unwise for us to bank on that unlikely event.
Don't miss any update on this topic
Create a free account and access your personalized content collection with our latest publications and analyses.
License and Republishing
World Economic Forum articles may be republished in accordance with the Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International Public License, and in accordance with our Terms of Use.
The views expressed in this article are those of the author alone and not the World Economic Forum.
Stay up to date:
Longevity Economy
Related topics:
Forum Stories newsletter
Bringing you weekly curated insights and analysis on the global issues that matter.
More on Equity, Diversity and InclusionSee all
Adam Amoussou and Angèle Melly Yanga
May 20, 2026