How to protect healthcare workers – and improve pandemic preparedness

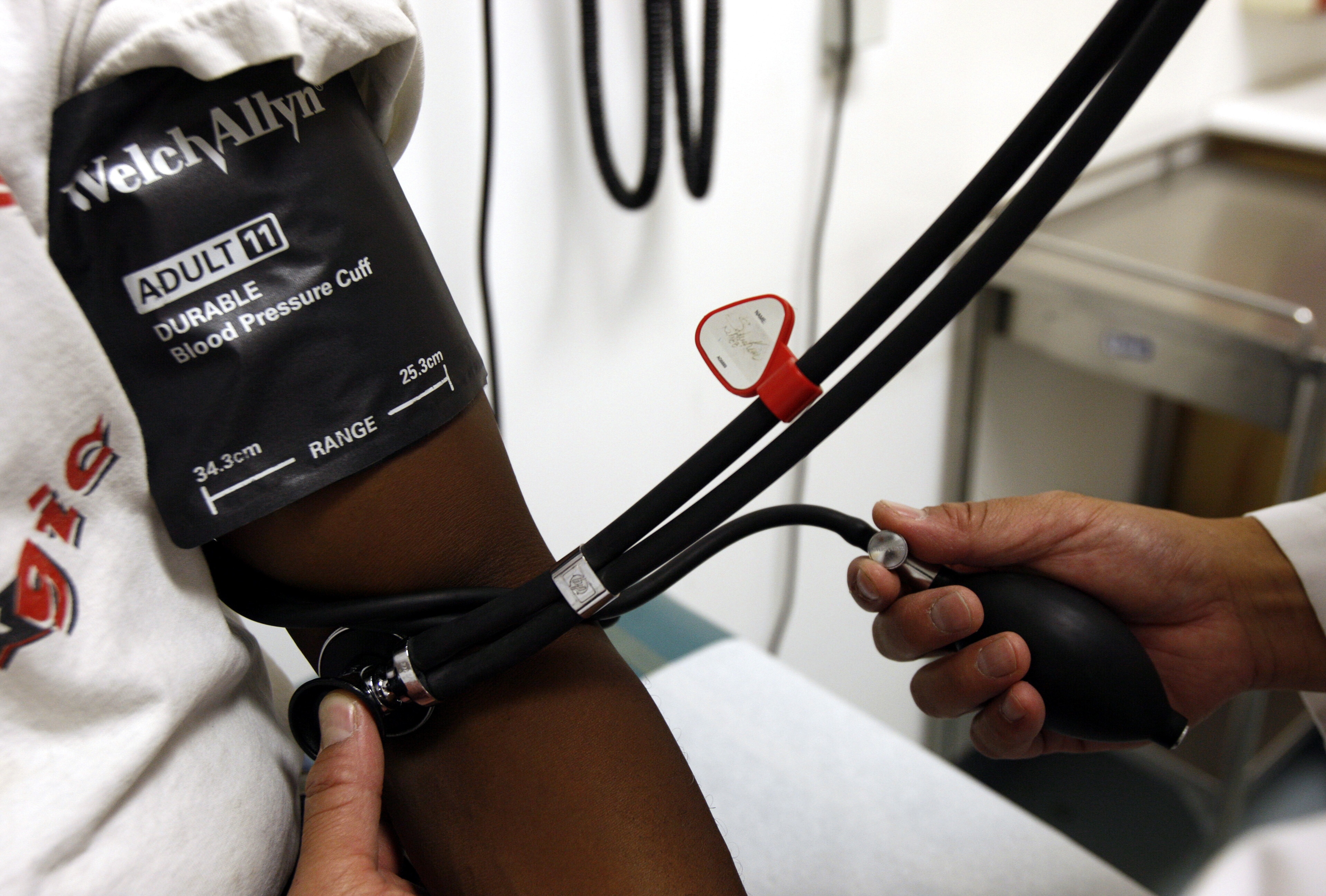
Healthcare workers are our greatest assets in fighting a pandemic. Here’s how we can support them. Image: REUTERS/Susana Vera
Listen to the article
- COVID-19 exacerbated the global shortage of healthcare workers and the challenges they face.
- With women representing 70% of the healthcare workforce, gender-based policies are needed to protect and support them.
- By improving healthcare working conditions and investing in our health workforce, we can better prepare for the next pandemic.
Worldwide, the COVID-19 pandemic underscored the structural vulnerabilities and lack of pandemic preparedness in our health systems.
These vulnerabilities were further impacted by a shortage of healthcare workers.
Have you read?
The pandemic brought an unprecedented demand for healthcare capacity in clinics, hospitals, intensive care units and home-care. Healthcare workers were providing care at significantly longer hours in overwhelmed facilities, frequently with insufficient skills and training combined with a lack of protective equipment. With facilities understaffed, many workers were double-shifting as caregivers and providing clinical training to volunteers.
The stressful working conditions have had a negative impact on healthcare workers’ physical, intellectual and psychological capacity to continue working in the sector. There is predicted to be a high turnover rate among healthcare workers, especially those in direct patient care and working in overwhelmed facilities.
Have you read?
This is not only detrimental to the workers themselves. Healthcare workers will remain our greatest asset for combating COVID-19 to the end as providers of vaccinations, as well as dealing with other global health risks through health advocacy, prevention, treatment and patient care. Failing to solve the problems with healthcare working conditions and the pressures these workers face could be detrimental to our capacity for dealing with future health emergencies.
Women are key to health security
During a World Economic Forum discussion, The Critical Role of Healthcare Workers during the Pandemic, Dr. Githinji Gitahi, Group CEO of Amref Health Africa, pointed out that as 70% of the global health workforce, women play a critical role in health security.
At the same time, the COVID-19 pandemic has disproportionally affected women. There has been a higher prevalence of COVID infections as well as anxiety, fear and suicide among female healthcare workers, compounded by the burden of home care that typically falls to women.
Responding to shocks in the healthcare environment made working conditions even more complex. Dr. Jennifer White, Director of the Health Emergency Department at Jefferson Health in Philadelphia, Pennsylvania, shares that the greatest challenge was the fear of the unknown – what is the virus, how it spreads and how to treat it.
This fear was compounded by the daily work experiences. The Jefferson Emergency Department was receiving 220 patients per day and nursing homes were devastated. Meanwhile, while caring for patients, workers had anxiety about how to protect their families, too, explains Dr. White.
To strengthen health systems and prepare for the next pandemic, it’s clear we need gender-based policies that will protect and improve the conditions of female healthcare workers.
6 steps to improving healthcare working conditions and pandemic preparedness
1. Prepare and invest. Despite repeated warnings that we could face a health pandemic in the near future, no country or health service was prepared. Healthcare should be reimagined based on the challenges faced during the COVID-19 pandemic – and healthcare workers should be leading health policy work. More investment is required for building resilient healthcare systems and facilities, leveraging communities and focusing healthcare work on prevention.
2. Address the nurse shortage and skills shortage in the health workforce. Every country reported a health workforce shortage. Empowering healthcare workers through training and building pipeline of workers is key, and doing so in a timely and accessible manner will alleviate overwhelmed facilities and enable better health responsiveness.
3. Prioritise the safety of healthcare workers. At the onset of the pandemic, a great number of healthcare workers did not have enough Personal Protective Equipment (PPE). The International Council of Nurses “believes that on average around 10% of all confirmed COVID-19 infections are among healthcare workers, with a range of 0-15%. At the time of reviewing data, more than 90 million people had been infected with COVID-19”. Inadequate safety in healthcare work environments, including the lack of PPE, compromised the health and safety of healthcare workers, their families and patients.
4. Compile comprehensive and systematic health data. Health data is crucial for providing the best healthcare response as well as to understand and respond to transmission of infection. During the pandemic, the lack of comprehensive data – and countries not recording health data in a systemic manner – resulted in slow turnaround times and a backlog of patients, worsening overwhelmed facilities.
5. Support the mental health needs of healthcare workers. Fighting a novel virus, responding to an influx of patients, working in fragile and overwhelmed settings and limiting contact with families and loved ones are just some of the challenges negatively affecting the psychological well-being of healthcare workers. Many healthcare workers reported the difficult working conditions as causes of stress, anxiety and depression, which is further worsened by personal and professional bias.
6. Take a cross-governmental and multistakeholder approach. Health ministries alone cannot solve the challenges with working conditions in the healthcare sector – an all-government approach is required. It is also important to leverage expertise from multiple stakeholders in order to drive transformational change in building safe, secure and responsive healthcare working environments.
Don't miss any update on this topic
Create a free account and access your personalized content collection with our latest publications and analyses.
License and Republishing
World Economic Forum articles may be republished in accordance with the Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International Public License, and in accordance with our Terms of Use.
The views expressed in this article are those of the author alone and not the World Economic Forum.
Stay up to date:
Pandemic Preparedness and Response
Related topics:
Forum Stories newsletter
Bringing you weekly curated insights and analysis on the global issues that matter.
More on Health and Healthcare SystemsSee all
Shyam Bishen
May 8, 2026