How ‘One World, One Health’ can move beyond a slogan to become a shared reality

A farmer near Pursat, Cambodia. International organizations are developing solutions to protect people and animals from infectious disease in a highly interconnected world. Image: WHO / Yoshi Shimizu
- No single discipline, sector or country can manage the threat of infectious disease alone in a highly interconnected world.
- This idea is the basis of the One Health initiative, created by international bodies to strengthen global cooperation on health.
- More can be done to tackle the effects of emerging zoonotic diseases (those originating in animals), antimicrobial resistance and climate change.
“Between animal and human medicine, there are no dividing lines – nor should there be.”
Rudolf Virchow, the German physician widely regarded as the father of modern pathology, made that declaration in 1856 against a backdrop of multiple global and regional health crises.
The third cholera pandemic (1846-1860), had originated in India and was engulfing swathes of Asia, Europe, Africa and North America, eventually killing well over 1 million people. An outbreak of trichinosis, a parasitic infection caused by eating raw or undercooked meat, sickened thousands in Europe, causing hundreds of deaths. And typhus, an often-fatal bacterial disease transmitted via infected fleas, lice or mites, had ravaged areas with poor hygiene, poverty and overcrowding in 1848.
These events convinced Virchow that diseases were just as much social and environmental issues as they were biological.
In the mid-19th century, the nexus between animal, human and ecosystem health was clear to Virchow. But it wasn’t until some 150 years later that the modern-day “One Health” concept took shape. It was articulated by the Manhattan Principles of 2004 following the 2003 global SARS outbreak, which was triggered by a novel coronavirus harboured by horseshoe bats.
The core message of the principles was that no single discipline or sector can properly manage the threat of disease in a globalized world. A trans-disciplinary, multisectoral approach that includes environmental health as a key component of human and animal health is essential.
Building on the Manhattan Principles, international organizations began formalizing the One Health collaboration. This led to the One Health Quadripartite of today, comprising the World Health Organization, the UN Food and Agriculture Organization, the UN Environment Programme and the World Organization for Animal Health.
The growing threat of infectious disease
The advocacy platform of the quadripartite has never been more urgent. Over 60% of known infectious diseases and up to 75% of emerging diseases originate in animals. Each year, on average, these so-called zoonotic diseases affect more than 2 billion people and claim over 2 million lives. And 600 million people fall ill from foodborne diseases each year, incurring an estimated $110 billion in medical expenses annually and huge productivity losses in low- and middle-income countries.
Antimicrobial resistance (AMR – when drugs stop being effective in treating a range of diseases) could cause 10 million deaths annually by 2050, with global economic costs reaching $100 trillion. In the Western Pacific, a projected 5.2 million deaths will be caused by drug-resistant infections between 2020 and 2030. AMR is expected to cost the region $148 billion in economic losses during this time, along with 172 million additional hospital days by 2030, taxing the region’s already-stretched health systems.
As one of the most climate-vulnerable regions globally, 3.5 million deaths occur in the Western Pacific each year from preventable environmental causes such as air pollution, unsafe water and extreme weather. Outdoor air pollution alone causes one death every 14 seconds.
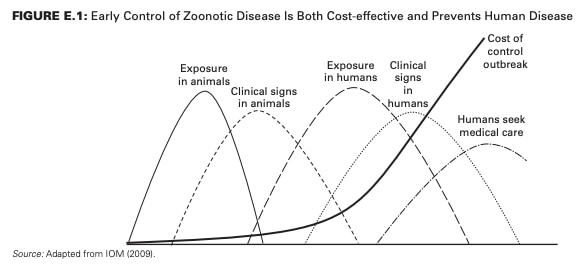
The One Health investment case
Countries in the Western Pacific region realize they need to act, both individually and collectively, to address infectious diseases.
Indonesia is working to reduce risks from certain zoonotic diseases. Heightened surveillance of avian influenza is being carried out at traditional poultry markets, for example. Efforts to control a climate-sensitive disease called leptospirosis are being strengthened in coastal and low-lying areas. Rabies, endemic in 26 of the country’s 38 provinces, is being addressed through accelerated animal vaccination, advanced surveillance and case management of rabid animals, and amplified risk communication at the community level.
Hit last year by a five-month dengue outbreak with 900 cases and three deaths, the island country of Tonga convened the Pacific’s first National Bridging Workshop, bringing together government and civil society organizations representing the human, animal and environmental health sectors to break silos and collaborate on preparing for, and responding to, vector-borne and other diseases.
Malaysia has been strengthening its AMR outbreak response in hospitals by training staff and updating national guidelines. It is boosting AMR surveillance capacity and drumming up political support across ministries beyond health.
But the painful lessons of COVID-19 have underscored that a piecemeal approach to One Health simply doesn’t work. Working to prevent pandemics through a comprehensive One Health approach would cost $10-11 billion per year globally, according to the World Bank. By comparison, managing and responding to pandemics would cost around $30 billion – three times as much as prevention.
The return on investment is even more compelling. Investing wisely in broader One Health prevention can deliver returns of up to 86%, and 3.4 billion dollars in annual investments could generate up to $30 billion in benefits.
Despite this mounting body of evidence, it’s been a challenge to secure consistent government funding for One Health initiatives. Policy-makers and budget holders, facing competing demands, are under pressure to demonstrate a quick fix. But the return on One Health investment is manifested in the longer term.
One Health as a political unifier
There is a potential game-changer for tackling infectious disease, however. The landmark Pandemic Agreement reached by WHO Member States in 2025 formally codifies One Health as key to avoiding pandemics. Once a country ratifies the Pandemic Agreement, it becomes legally binding, making it incumbent on that government to fully support One Health.
Still, will all of this really happen at a time when health budgets are shrinking and being diverted to other areas such as militarization and defence?
As a former parliamentarian and Health Minister of my homeland Tonga, I know full well that all health is ultimately political. For One Health to succeed and be sustained, political leaders and policy-makers at the very highest levels must recognize how essential it is for health and national security – and act.
From 5-7 April 2026, the French government is hosting a One Health Summit in Lyon. It will convene WHO Member States, several represented by presidents and prime ministers, alongside ministers of health, finance and other portfolios. At a time of fraying multilateralism, this gathering symbolizes that where there’s political will there’s usually a way.
The Lyon One Health Summit could be a unifier. It could facilitate regional and global collaboration between countries, as well as multisectoral collaboration within countries. This could lead to sustainable financing to implement One Health-related programmes to tackle infectious disease.
This is a very real opportunity to prove that One World, One Health – the vision with its roots in the work of Rudolf Virchow a century ago – can be more than a slogan. It can represent a shared reality we can, and should, commit to for once and for all.
Don't miss any update on this topic
Create a free account and access your personalized content collection with our latest publications and analyses.
License and Republishing
World Economic Forum articles may be republished in accordance with the Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International Public License, and in accordance with our Terms of Use.
The views expressed in this article are those of the author alone and not the World Economic Forum.
Stay up to date:
Pandemic Preparedness and Response
Related topics:
Forum Stories newsletter
Bringing you weekly curated insights and analysis on the global issues that matter.
More on Health and Healthcare SystemsSee all
Naoko Tochibayashi
April 2, 2026