Why closing the women’s health gap starts with how care is delivered
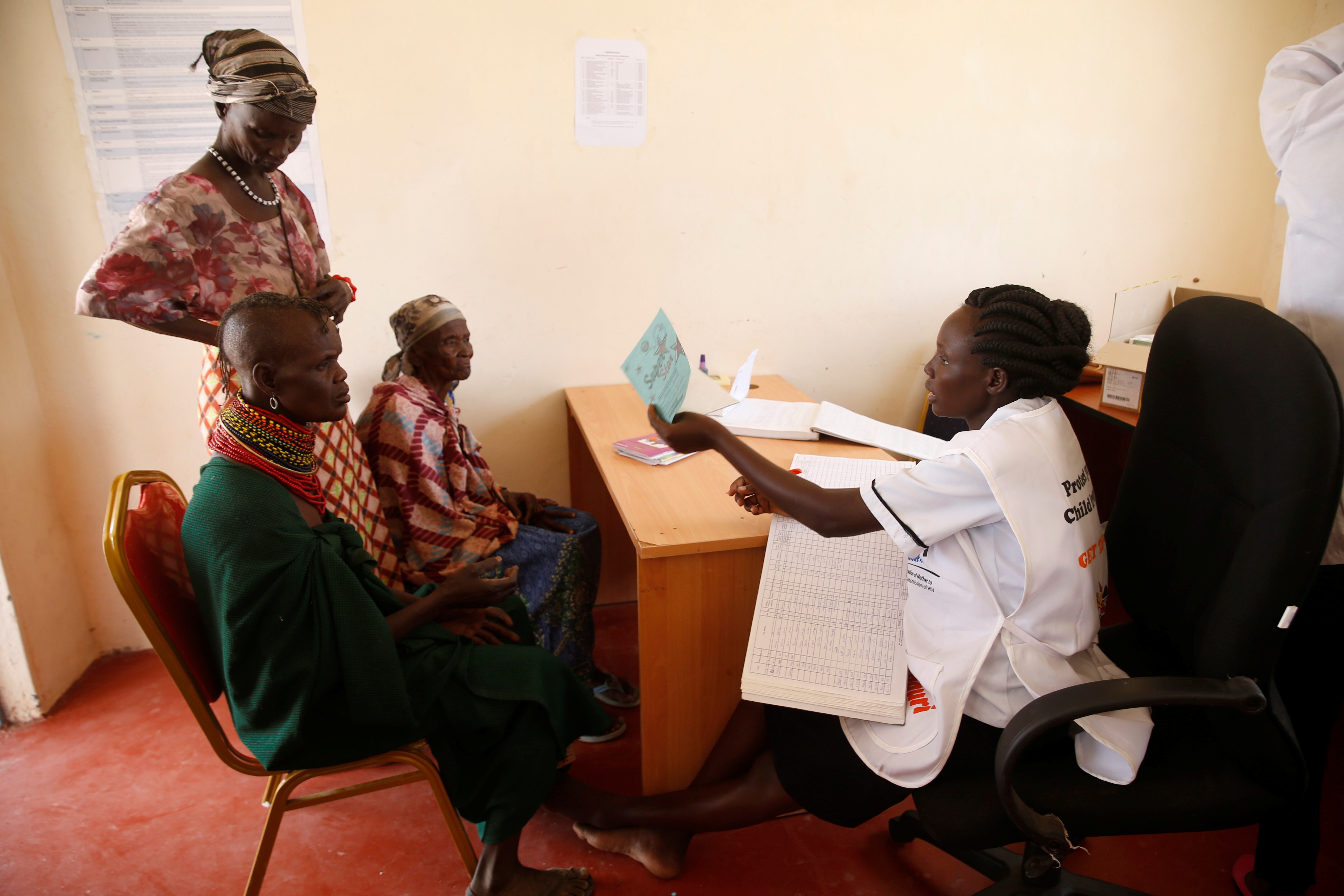
Digital tools help reduce the women’s health gap but work best with trusted community health workers Image: REUTERS/Baz Ratner
- Many women’s health conditions are preventable or manageable but healthcare systems often fail to deliver accessible, affordable and continuous care that fits women’s real-life circumstances.
- Community-led health models, such as in India, Brazil and Kenya, demonstrate how women receive better care when services are local, trusted and relationship-based, especially in underserved communities.
- Digital tools such as telemedicine and remote monitoring can improve access and follow-up to reduce women’s health gaps but work best with trained community health workers.
Women’s health is often discussed in terms of research, funding or awareness. All three matter. However, the persistence of the women’s health gap points to another challenge: many health systems are still not designed around how women actually access care.
The scale of the gap is now well documented. Research from the World Economic Forum and McKinsey Health Institute found that women spend 25% more of their lives in poor health than men and that closing this gap could add at least $1 trillion to the global economy annually by 2040.
The Forum’s Blueprint to Close the Women’s Health Gap reinforces the same point: improving women’s health is not only a clinical priority but an economic and social one.
This issue is becoming more urgent as health systems face rising costs, workforce shortages and growing pressure to deliver care beyond overstretched hospitals. Many conditions driving poor health among women are not beyond medical understanding.
Anaemia, maternal complications, cervical cancer and chronic diseases can often be prevented, detected early or managed with timely care.
Yet access remains uneven. According to the World Health Organization, about 260,000 women died during and following pregnancy and childbirth in 2023, with most deaths preventable. WHO also estimates that 30% of women aged 15-49 and 37% of pregnant women are affected by anaemia.
The question, then, is not only whether better solutions exist. It is whether health systems are able to deliver them consistently, affordably and close to where women live.
Community-led health systems do not replace hospitals, specialists or formal clinics; they extend their reach by building trusted links between households and care providers.
”Healthcare delivery is the bottleneck
Healthcare innovation has accelerated rapidly, from digital diagnostics to telemedicine and new models of care. Yet, innovation alone does not guarantee access.
For many women, especially in rural or low-resource settings, the barriers are practical and social: distance from facilities, out-of-pocket costs, lack of childcare, restrictive norms, limited awareness or weak follow-up.
This is not only a Global South issue. Deloitte’s analysis found that employed women in the United States face higher annual out-of-pocket healthcare costs than employed men, even when pregnancy-related expenses are excluded.
This suggests that the women’s health gap is not simply about a lack of medical knowledge. It is also about whether care pathways are reachable, affordable, trusted and designed around women’s realities.
A woman may know she needs antenatal care but be unable to travel regularly. A girl may need anaemia screening but never come into contact with the formal health system. A woman eligible for cervical cancer screening may delay care because services are too far away, intimidating or poorly explained.
In each case, healthcare availability and delivery remain the issue.
Community systems already show what works
Community-led health systems do not replace hospitals, specialists or formal clinics; they extend their reach by building trusted links between households and care providers.
India’s network of Accredited Social Health Activists (ASHAs) offers one of the most visible examples of this model. More than one million ASHAs connect communities with the health system, particularly in rural and underserved areas.
The World Health Organization has recognised their role in improving access to primary healthcare and linking households with essential services.
Their contribution is especially relevant for women’s health. ASHAs support antenatal care, immunization, family planning, health education and referrals. Their strength ultimately lies in the trust they build as they are the known faces who understand local barriers and can follow up over time.
Similar lessons can be seen elsewhere. Brazil’s Family Health Strategy uses community health workers as part of primary care teams that conduct home visits, provide preventive care and connect families to the broader health system. Kenya’s Community Health Strategy 2020-2025 is built around bringing health services closer to households through community health units linked to facilities.
The details differ across countries. However, the underlying lesson is similar: women’s health improves when care is local, continuous and trusted.
Community health systems often rely on women frontline workers whose labour is undervalued, many of whom carry heavy workloads, limited pay and unclear career pathways.
”Technology works best when it strengthens human systems
Digital tools can make these models more powerful. Mobile health platforms, teleconsultations and digital records can help frontline workers track pregnancies, identify high-risk cases, send reminders and connect women to higher levels of care.
However, technology should not be treated as a substitute for community trust. A digital tool cannot accompany a woman to a clinic, notice when she has missed multiple visits or understand the family and social pressures shaping her choices. Frontline workers often provide the human continuity that technology alone cannot deliver.
This is where investment in women’s health innovation needs to be better connected to delivery systems. BCG’s work with the World Economic Forum identifies high-potential opportunities such as virtual women’s healthcare and remote maternal health monitoring. But these tools will only matter if they are connected to trusted delivery channels.
The workforce must not remain invisible
There is, however, a tension that cannot be ignored. Community health systems often rely on women frontline workers whose labour is undervalued, many of whom carry heavy workloads, limited pay and unclear career pathways.
If countries want community-led systems to close the women’s health gap, they must invest in the people who make these systems work. That means better training, fair compensation, supervision, safety and formal recognition within national health strategies.
This is also a resilience issue. The Partnership for Health System Sustainability and Resilience assesses health systems through domains such as governance, financing, workforce, service delivery, medicines and technology, population health and environmental sustainability.
Community health workers sit directly at this intersection. WHO also projects a global shortfall of 11 million health workers by 2030, mostly in low- and lower-middle-income countries.
In that context, community health workers should not be seen as peripheral volunteers or temporary programme staff. They are part of the core infrastructure of resilient health systems.
Community healthcare is beneficial beyond the Global South
The relevance of community-led models is also relevant to high-income countries struggling with rising healthcare costs, ageing populations, workforce shortages and declining access to primary care in rural areas. The idea is to redesign care so it reaches people earlier, closer to home and with greater continuity.
For women’s health, this shift is particularly urgent. The gap in care doesn’t come from a single lapse but from repeated failures to engage, screen, refer or follow up with women on their health. Community-led delivery can close those gaps before they become crises.
Closing the women’s health gap will require more research, more investment and better policy but it will also require a more practical question: how does care actually reach women?
The answer may not lie only in laboratories or hospitals but in the community, where trust is built, prevention begins and health systems meet women where they are.
Don't miss any update on this topic
Create a free account and access your personalized content collection with our latest publications and analyses.
License and Republishing
World Economic Forum articles may be republished in accordance with the Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International Public License, and in accordance with our Terms of Use.
The views expressed in this article are those of the author alone and not the World Economic Forum.
Stay up to date:
Women's Health
Forum Stories newsletter
Bringing you weekly curated insights and analysis on the global issues that matter.
More on Health and Healthcare SystemsSee all
Shyam Bishen
May 8, 2026