Mimicking coronavirus could be key for a COVID-19 vaccine

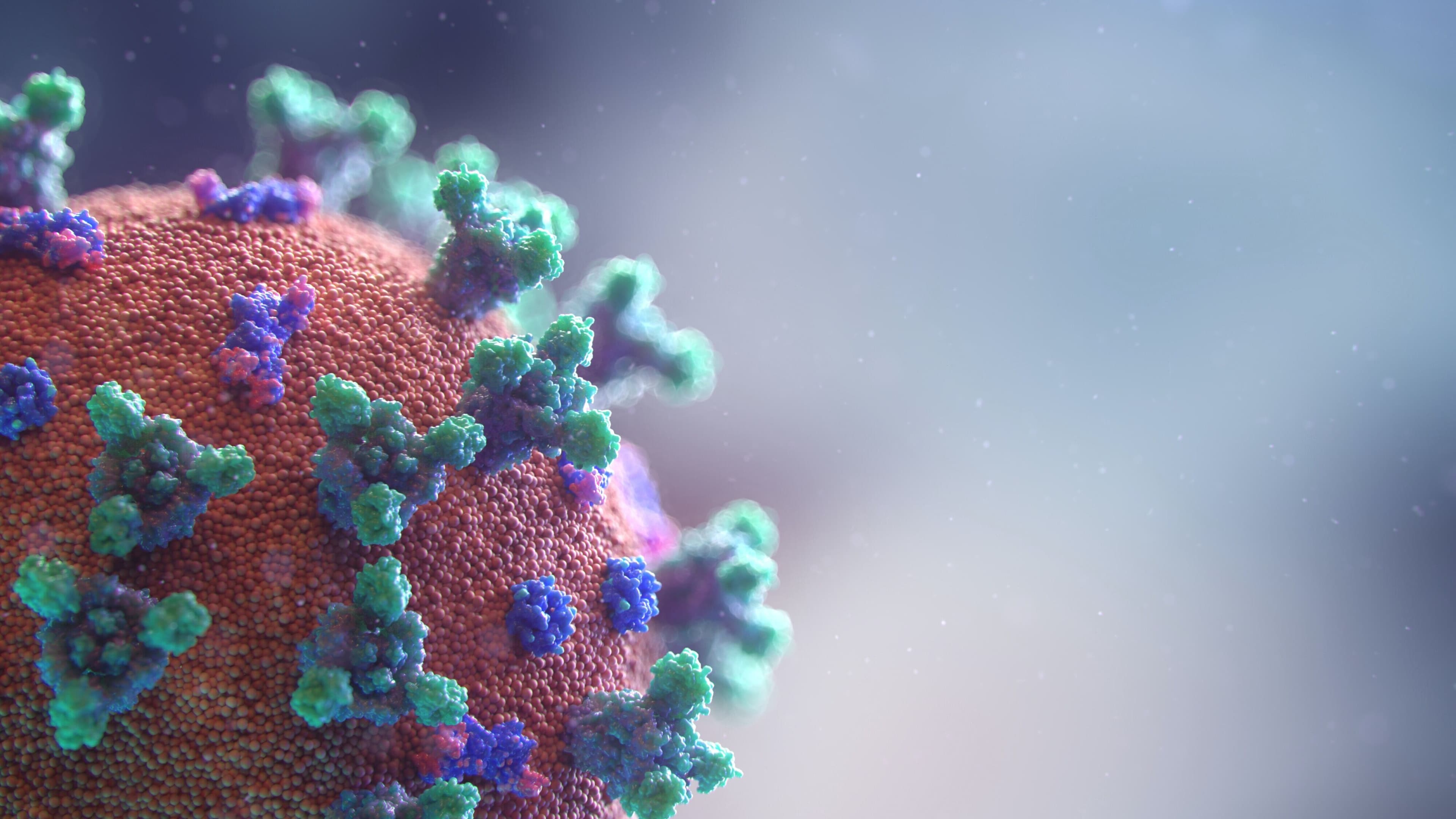
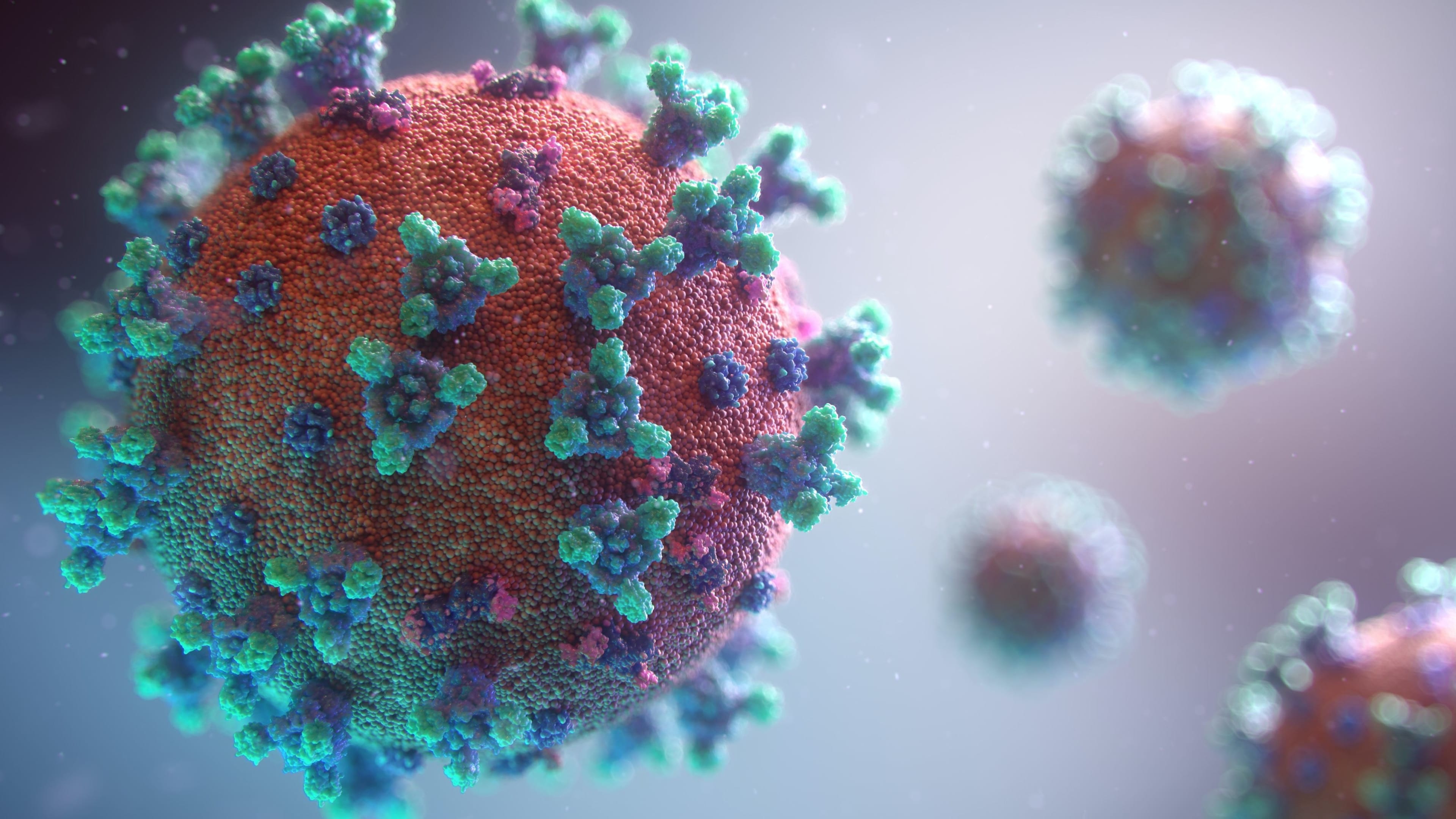
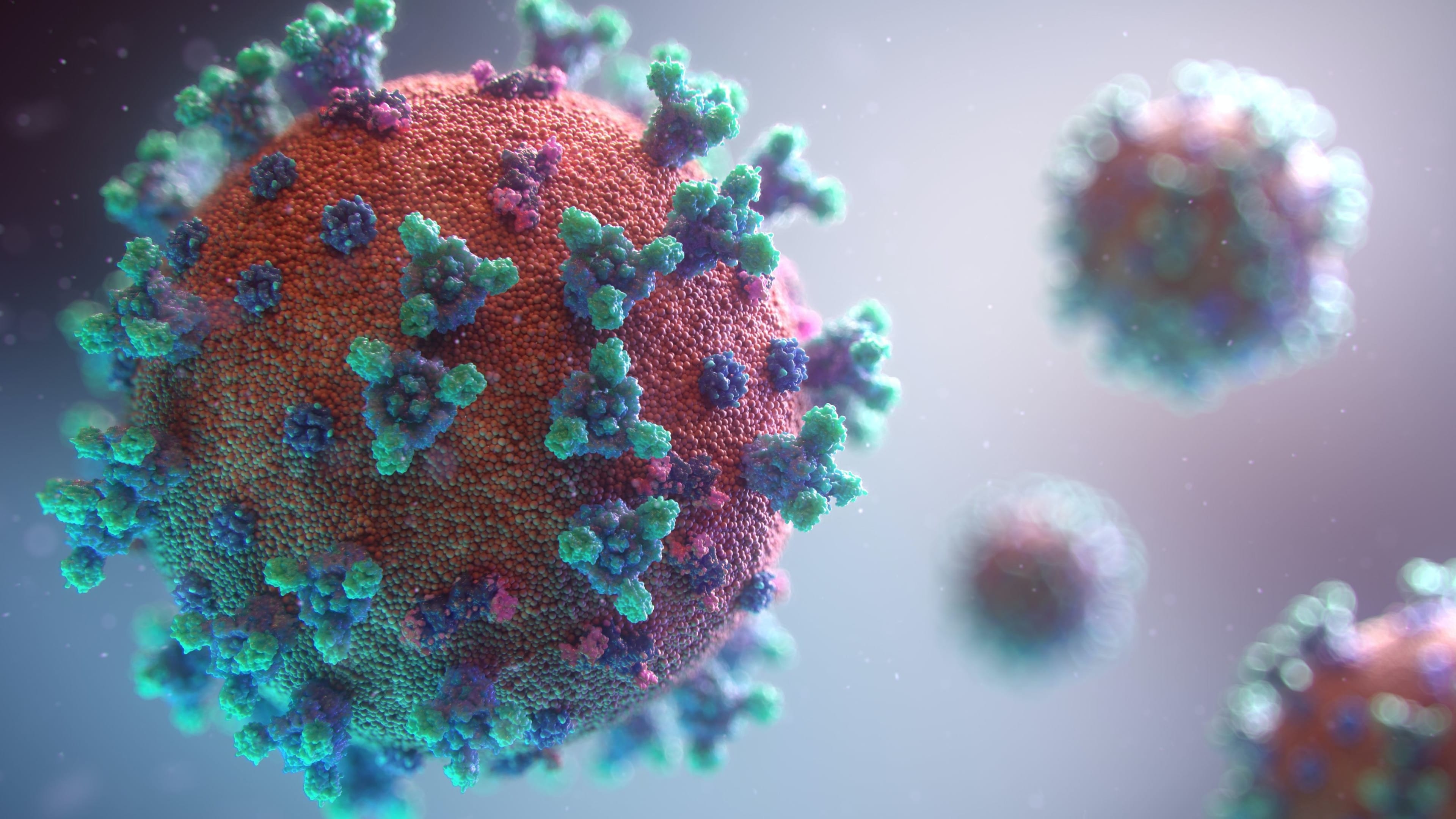
Hundreds of vaccines against COVID-19 are being developed across the world. Image: REUTERS/Maxim Shemetov

Explore and monitor how COVID-19 is affecting economies, industries and global issues

Get involved with our crowdsourced digital platform to deliver impact at scale
Stay up to date:
COVID-19
- A new technique could help increase the effectiveness of a COVID-19 vaccine, according to new research.
- It works by designing the vaccine so that it partially mimics the structure of the virus.
- The research has been carried out by biomedical engineering department at the University at Buffalo with support of other institutions.
A new technique could help increase the effectiveness of vaccines against the novel coronavirus, the virus that causes COVID-19, researchers report.
One solution to the problem of creating an effective COVID-19 vaccine might lie in designing vaccines that partially mimic the structure of the virus, says Jonathan F. Lovell, associate professor in the biomedical engineering department at the University at Buffalo.
One of the proteins on the virus—located on the characteristic COVID spike—has a component called the receptor-binding domain, or RBD, which is its “Achilles heel.” That is, Lovell says, antibodies against this part of the virus have the potential to neutralize the virus.
It would be “appealing if a vaccine could induce high-levels of antibodies against the RBD,” Lovell says. “One way to achieve this goal is to use the RBD protein itself as an antigen, that is, the component of the vaccine that the immune response will be directed against.”
The team hypothesized that by converting the RBD into a nanoparticle (similar in size to the virus itself) instead of letting it remain in its natural form as a small protein, it would generate higher levels of neutralizing antibodies and its ability to generate an immune response would increase.
Lovell’s team had previously developed a technology that makes it easy to convert small, purified proteins into particles through the use of liposomes, or small nanoparticles formed from naturally-occurring fatty components. In the new study, the researchers included within the liposomes a special lipid called cobalt-porphyrin-phospholipid, or CoPoP. That special lipid enables the RBD protein to rapidly bind to the liposomes, forming more nanoparticles that generate an immune response, Lovell says.
The team observed that when they converted the RBD into nanoparticles, it maintained its correct, three-dimensional shape and the particles were stable in incubation conditions similar to those in the human body. When laboratory mice and rabbits were immunized with the RBD particles, high antibody levels were induced. Compared to other materials that are combined with the RBD to enhance the immune response, only the approach with particles containing CoPoP gave strong responses.
Other vaccine adjuvant technology doesn’t have the capacity to convert the RBD into particle-form, Lovell says.
“We think these results provide evidence to the vaccine-development community that the RBD antigen benefits a lot from being in particle format,” Lovell says. “This could help inform future vaccine design that targets this specific antigen.”
The paper appears in Advanced Materials. Additional coauthors are from Texas Biomedical Research Institute, Penn State, McGill University, the US Centers for Disease Control and Prevention, and the University at Buffalo.
The National Institutes of Health and McGill University supported the work.
Source: University at Buffalo
Don't miss any update on this topic
Create a free account and access your personalized content collection with our latest publications and analyses.
License and Republishing
World Economic Forum articles may be republished in accordance with the Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International Public License, and in accordance with our Terms of Use.
The views expressed in this article are those of the author alone and not the World Economic Forum.
The Agenda Weekly
A weekly update of the most important issues driving the global agenda
You can unsubscribe at any time using the link in our emails. For more details, review our privacy policy.
More on COVID-19See all
Charlotte Edmond
January 8, 2024
Charlotte Edmond
October 11, 2023
Douglas Broom
August 8, 2023
Simon Nicholas Williams
May 9, 2023
Philip Clarke, Jack Pollard and Mara Violato
April 17, 2023