Why ovarian cancer must be part of the global cancer response

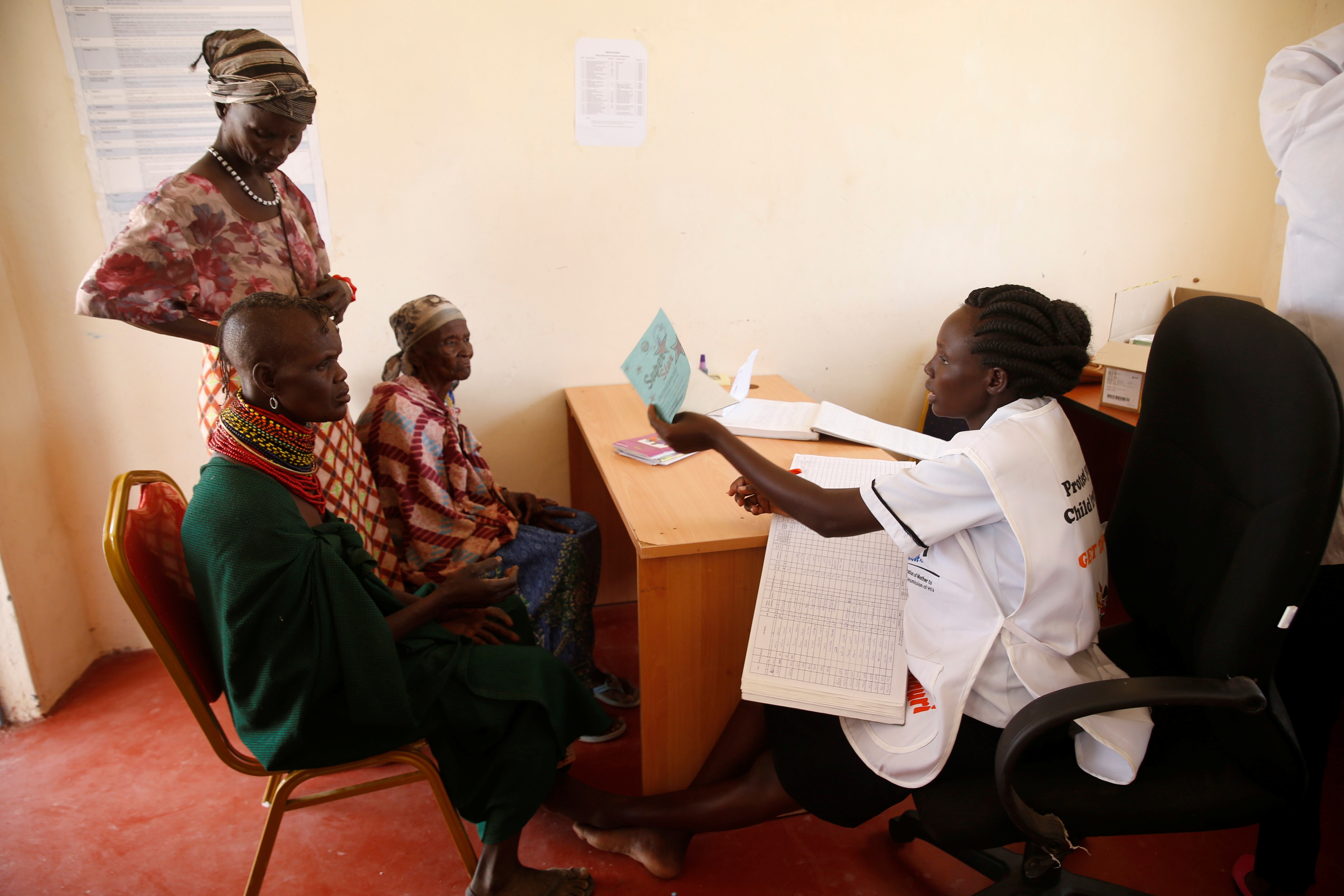
World Ovarian Cancer Day is an opportunity to integrate ovarian cancer into wider global cancer response efforts. Image: REUTERS/Maxim Shemetov
- For every 10 women diagnosed with ovarian cancer, approximately seven will die – a mortality rate higher than any other major women's cancer.
- Integrating ovarian cancer into existing global health frameworks could save 2.5 million lives by mid-century – without requiring new programmes.
- This World Ovarian Cancer Day was a moment to integrate ovarian cancer into the wider global push to reduce the impact of cancer on women worldwide.
Every minute, seven women are diagnosed with one of the four major women's cancers: breast, cervical, uterine or ovarian. By 2050, that number will rise to eleven. While global cases are set to rise by 53%, the increase in low- and lower-middle-income countries is forecast at 151% and 82% respectively. Without a change in course, more than 51 million women will die by mid-century. That is a toll seven times larger than reported COVID-19 deaths.
The world has begun to respond. The World Health Organization's Global Breast Cancer Initiative and Cervical Cancer Elimination Initiative are catalyzing national plans, mobilizing investment and setting mortality reduction targets that hold systems accountable. These achievements are already beginning to reshape how countries approach women's cancer control.
Hot on the heels of World Ovarian Cancer Day (WOCD) last week, we have the opportunity to accelerate that progress by building on what works, and expanding proven models to ensure ovarian cancer is no longer left behind.
Why does ovarian cancer have more deaths per woman diagnosed?
Of the four major women's cancers, ovarian cancer sees more deaths per woman diagnosed than any other. For every ten women diagnosed, approximately seven will die. This is not primarily a reflection of the disease's biology; it is a consequence of how women experience it within health systems that were not designed with it in mind.
Ovarian cancer is frequently diagnosed late. Its symptoms, such as bloating, persistent pelvic pain and changes in appetite, are non-specific and frequently overlooked or mistaken for less serious conditions. There is no population-wide screening test. Prevention through vaccination is not possible. Outcomes depend almost entirely on seeking help early, timely referral, surgical expertise and access to treatment.
The World Ovarian Cancer Coalition's Every Woman Study, first conducted in 2018, provided the first large-scale global insights into how women experience ovarian cancer. The subsequent Every Woman Study: Low- and Middle-Income Edition, published in The Lancet Obstetrics, Gynaecology & Women's Health across 22 countries, captures experiences in settings where most of the world’s women live.
The findings are consistent and stark. Women face low awareness of symptoms, long delays in diagnosis and significant barriers to accessing care.
Among the women who participated in the low- and middle-income edition, not even one had accessed a PARP inhibitor, a treatment that extends survival and is standard of care in many high-income settings.
These challenges are not unique to ovarian cancer, but they are particularly consequential for it. They are system failures global initiatives are addressing for breast and cervical cancer through awareness, referral pathways, diagnostic capacity and treatment access. Without deliberate inclusion in global frameworks, ovarian cancer will continue to be underserved. Not because we lack the tools, but because we have not yet chosen to apply them consistently.
The price of inaction on ovarian cancer
The implications extend beyond health outcomes. The World Ovarian Cancer Coalition's Socioeconomic Burden of Ovarian Cancer study, published in JCO Global Oncology, found that in 2023 the economic losses from ovarian cancer across just eleven countries totalled $70 billion. Every woman lost to ovarian cancer is a mother, caregiver, income earner and community contributor. Reducing avoidable mortality has direct effects on workforce participation, household stability and broader economic resilience. These are effects that compound across generations.
At the same time, the opportunity for action is quantifiable. The Global Breast Cancer Initiative is built around a 2.5% annual mortality reduction target. Applying the same modest target to ovarian cancer could save 2.5 million lives between now and 2050. Crucially, this would not require new vertical programmes. It would mean extending existing investments in awareness, diagnosis, referral pathways and treatment access that are already being built for breast and cervical cancer. Advances in treatment, including targeted therapies that have transformed outcomes for some women with ovarian cancer, remain out of reach for the majority of the world's women.
A more integrated approach to women's cancer frameworks creates the conditions for those advances to translate into outcomes at scale, particularly in the settings where need is greatest and systems are evolving fastest.
What integration looks like in practice
Women do not move through health systems one cancer at a time. They navigate a single continuum of care with shared entry points, shared barriers and shared needs. Cancer strategies should reflect that reality rather than fragment it. In practice, this means expanding the scope of existing global frameworks to reflect the full spectrum of women's cancers; aligning indicators and targets across cancers where health system pathways overlap; leveraging current investments to strengthen diagnosis and treatment for multiple cancers simultaneously; and continuing to build the evidence base, particularly from lower-income settings, to guide policy and financing decisions.
The breast cancer experience offers a template. In many low- and middle-income countries, coordinated efforts between governments, global health organizations and industry partners have shown that combining diagnostic capacity building, patient navigation and access to treatment can translate global frameworks into real improvements in outcomes. Partnerships supporting the World Health Organization’s Global Breast Cancer Initiative, including contributions from organizations such as Roche, demonstrate how these elements can come together in practice. The same logic applies to ovarian cancer. Such an approach would not dilute existing efforts. It would extend their reach, improve efficiency and multiply their impact, making integration not only necessary, but cost-effective.
This World Ovarian Cancer Day is a moment to act
As the world reflects on World Ovarian Cancer Day, the opportunity is clear. The evidence is in place, the systems are evolving and the frameworks that could extend progress to ovarian cancer already exist. Integrating ovarian cancer into global women's cancer strategies is not a distant ambition. It means naming it in targets, embedding it in national cancer plans, holding systems accountable and ensuring it shapes the investment decisions that follow. That is a practical next step that global health leaders, funders and governments are well positioned to take. Millions of women around the world are counting on them to do so.
The Global Alliance for Women's Health is leading the charge to close the women’s health gap, mobilizing resources and fostering innovation across a range of critical conditions. By mobilizing resources and encouraging public private sector collaboration to improve research, data collection and policy attention, the Alliance aims to ensure that no woman is left behind in the fight against cancer.
Closing the ovarian cancer care gap is not only a health imperative – it is a driver of economic and social well-being for families and societies worldwide.
Don't miss any update on this topic
Create a free account and access your personalized content collection with our latest publications and analyses.
License and Republishing
World Economic Forum articles may be republished in accordance with the Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International Public License, and in accordance with our Terms of Use.
The views expressed in this article are those of the author alone and not the World Economic Forum.
Stay up to date:
Women's Health
Forum Stories newsletter
Bringing you weekly curated insights and analysis on the global issues that matter.
More on Health and Healthcare SystemsSee all
Gaurav Ghewade
May 11, 2026