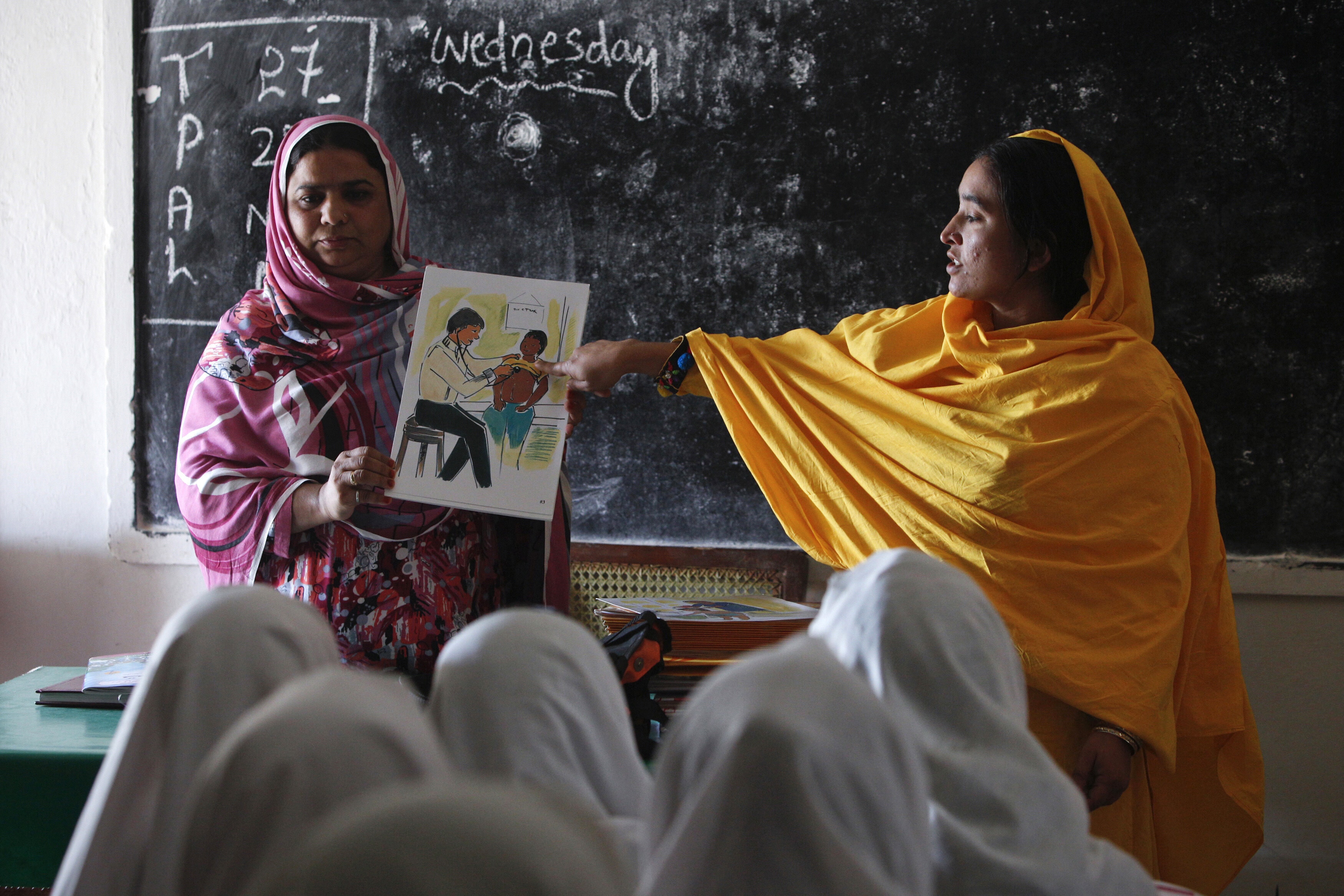In a world of medical miracles, we need to go the last mile

Digital technology can help to bring healthcare to remote locations Image: REUTERS/Goran Tomasevic
Imagine the following: you live in a rural community, and the nearest hospital is hours away. Your child falls seriously ill and your only choice is to spend most of the day trekking to the nearest health centre to wait in line while praying the drug you need is in stock that day. Millions of families across the globe don’t have to imagine this – it is their reality.
We live in an age of medical and technological miracles. Yet 6 million children still die each year for want of simple health solutions that cost less than a cup of coffee. This is a plague we have the power to prevent.
The world is experiencing the greatest health worker shortage in history lacking more than 7 million health workers (a number forecast to more than double to 18 million by 2030). We need more health workers and we need them fast. Doctors and nurses, while vital to healthcare systems, can’t meet the demand alone. Our current, century-old model for medical training is impossibly costly, so will never catch up with demand.

Today virtually every other sector – from books to retail and taxis – has been positively reinvented by mobile technology. Now it’s possible for technology to reinvent community healthcare on a game-changing scale by transforming ordinary villagers into life-saving community health workers. To meet the world’s basic health needs, we must build an army of digitally-empowered, community health workers.
The future of digital health
In Africa, the mobile phone leapt past copper cable, then mobile money leapt over retail banking. Now Last Mile Health and Living Goods, alongside longstanding partners like Medic Mobile and BRAC, are using mobile tools to help Africa rapidly reinvent health systems. These organizations use the disruptive power of mobile technology to empower thousands of community health workers who provide home delivery on demand for life-saving health products and services.
Digital powered community health workers deliver health services to families in their own neighbourhoods. Equipped with a new generation of health apps using artificial intelligence, these health workers can treat the most common deadly diseases, employ advanced field-based diagnostics, provide expert support for pregnancies and newborns, offer home-based family planning and track down under-immunized kids. Before mobile technology, you would need at least a four-year nursing degree to offer these services in most countries. The annual cost to support nurses can run from $5,000 to $100,000. With today’s technology, we can train community health workers in these life-saving skills in just a few short weeks, and support them for less than $2,000 per year. By taking advantage of digital technology, these frontline health workers have the potential to save millions of lives at a far faster and lower cost than ever before.
Remember the parent with the sick child? Now imagine this: instead of trudging to the health clinic to get help, you can call a nearby, digitally-empowered health worker equipped with a smartphone. She comes to your house and uses a simple mobile app to provide an accurate diagnosis and deliver life-saving medicine on the spot. Your child’s diagnosis and treatment rest in the palm of your health worker’s hand. For millions, this could mean the difference between life and death.
Saving lives and saving money
We believe it’s possible for mobile technology to extend life-saving care to millions of people. The benefits to society will be profound and far-reaching:
· Saving lives: A randomized control trial shows Living Goods health workers can reduce child mortality by over 25% at an annual cost of less than $2 per person reached. In Liberia, Last Mile Health’s approach increases the odds of kids receiving life-saving care by more than 50% and the proportion of mothers birthing in clinics to 82%. In partnership with governments and leading NGOs, Living Goods and Last Mile Health already serve 6 million people.
· Saving money: By harnessing mobile tools, health systems can train and deploy community health workers at a fraction of what it costs to train doctors and nurses. Community-delivered care dramatically reduces admittances to costly emergency rooms. Home-delivered care saves patients money too, eliminating transport costs and the income lost from travel and waiting time. The convenience of home delivery means patients seek care sooner and thus are much less likely to develop high-cost, acute conditions.
· Creating jobs: Across the globe, people fear that technology is destroying jobs, but digitally-empowered health delivery will do the opposite. By dramatically cutting the time it takes to train effective health workers, mobile technology helps to create thousands of new well-paying jobs in the health sector, launching a generation on career paths that would have been out of reach just a few years ago. Moreover, community health workers provide a 10:1 return on investment when increased productivity and economic activity are taken into account.
· Empowering women: More than 90% of these new health workers are women. Women community health workers in these countries are building their confidence, their financial independence and raising their status in their villages. So it’s no surprise that last year more than 50 community health workers in Uganda ran for public office and many of them won.
· Preventing pandemics: The increasing frequency of deadly epidemics like Ebola places the planet at grave risk of crisis-scale pandemics. The key to stopping the next pandemic is early detection. Using their mobile apps, health workers can report on disease vectors and unusual death rates in real time and enable public health systems to respond far faster, which lowers the odds of outbreaks flaring into epidemics.
· Strengthening health systems: Community health workers extend the reach of health systems to the most remote communities reaching previously underserved populations. For instance, following the West African Ebola epidemic, the Government of Liberia and its partners have rolled out a National Community Health Assistant Programme to deploy more than 4,000 paid, supervised community health workers to serve 1.2 million people. This approach, says Dr Ruhakana Rugunda, Prime Minister of Uganda, “solves two of our biggest challenges in the healthcare sector: how to keep vital medicines in stock, and how to compensate and retain community health workers.”
It took just a few short years for mobile phones to sweep across Africa. Now, organizations like Living Goods and Last Mile Health are using the disruptive power of mobile technology to empower thousands of community health workers to provide life-saving healthcare to the doorsteps of families in need, as and when they demand it. We now have the opportunity to scale this model in a historic way to meet the growing demand for healthcare around the world.
At the World Economic Forum’s Annual Meeting this year, we are launching an ambitious initiative to digitally equip nearly 50,000 community health workers across the globe. Combining Living Goods’ proven Smart Health app and home delivery model with a powerful new digital training solution from Last Mile Health’s Community Health Academy, we have the opportunity to extend quality care to the doorsteps of millions. With aid funding in decline, now is the time for a smart combination of philanthropy and business to step up and step forward to lead innovation in healthcare delivery.
Don't miss any update on this topic
Create a free account and access your personalized content collection with our latest publications and analyses.
License and Republishing
World Economic Forum articles may be republished in accordance with the Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International Public License, and in accordance with our Terms of Use.
The views expressed in this article are those of the author alone and not the World Economic Forum.
Stay up to date:
Global Health
Forum Stories newsletter
Bringing you weekly curated insights and analysis on the global issues that matter.
More on Health and Healthcare SystemsSee all
Matthew Oliver
March 24, 2026