Virtual health is helping hospitals deliver care anywhere. That's never been more important

Virtual health can help to ease burdens on health services worldwide and improve patient outcomes. Image: Seha Virtual Hospital
Abdulaziz Alhomod
Chief Innovation Officer, Seha Virtual Hospital, Ministry of Health of Saudi Arabia- Around 4.5 billion people cannot access essential health services - virtual health offers a scalable path to closing that gap.
- By 2030, healthcare's economic burden could reach $47 trillion, but technology can assist by reducing costs and improving care.
- Hospitals in public health authorities from Saudi Arabia to the US are implementing virtual health, providing case studies for others to follow.
Virtual health is redefining how care is delivered, shifting systems from episodic, facility-based models to continuous, patient-centred care that can reach people anywhere.
Scaling virtual health can accelerate progress toward universal health coverage, expanding access, improving efficiency and enabling better management of chronic conditions—especially in underserved populations.
Realizing this potential will require coordinated action, including interoperable digital infrastructure, aligned governance and investment, and sustainable financing models to ensure broader access and system-wide transformation.
Health ministers across every continent are facing intensifying health system pressures that are outpacing the capacity of existing models to respond. Today, the impact of these pressures ripple beyond the health sector, threatening labour markets, fiscal systems and economic productivity across societies.
The global healthcare challenge
Around 4.5 billion people cannot access essential health services, and by 2030 the global health workforce is projected to face a shortage of 11 million workers. Chronic conditions are driving up the cost of care and many national budgets are struggling to absorb these costs, with global health spending already reaching ~$10 trillion in 2021 – more than doubling since 2000. The global average cost of medical health benefits is projected to rise by 10.3% this year – following similar increases in 2025 and 2024 – with regional variation ranging from 8.2% in Europe to up to 14% in Asia Pacific.
These challenges are further compounded by growing shocks – from climate-related disruptions, to pandemics and geopolitical instability – that continue to test health system resilience.
Traditional healthcare delivery models were not engineered to absorb these conditions. Health systems remain largely organized around episodic, facility-based approaches, designed for populations with shorter life expectancies, predominantly acute conditions and limited flows of health information. However, these models are no longer equipped to meet the demand for continuous, coordinated care across populations with more complex health needs. This misalignment is increasingly at odds with the goals of universal health coverage, which require systems to deliver accessible, continuous and equitable care at scale.
How can technology improve global access to healthcare?
At the same time, a profound shift in how individuals engage with healthcare is underway. Digital tools and platforms are increasingly functioning as the front door to care – shaping how people access information, navigate systems and initiate services. Virtual consultations, remote monitoring, e-pharmacies and AI-enabled triage are becoming embedded in everyday care pathways. Every day, more than 40 million people turn to ChatGPT for health-related questions, while billions of queries are processed through search engines. Digital platforms now enable appointment booking, prescriptions and ongoing care beyond physical facilities.
Across the broader economy, those same technological forces are restructuring workforce dynamics. While other sectors embrace tech and AI-enabled operating models, healthcare continues to frame its central workforce challenge as a shortage of people. It is now time to explore how technology could fundamentally bridge key gaps in care delivery models. McKinsey Global Institute estimates that digital health interventions including remote monitoring, AI and automation could generate between $1.5 and $3 trillion in annual efficiency savings globally by 2030.
Despite significant investment, the scope and speed of systemic change has been slow. Many initiatives remain confined to pilots, limiting their ability to integrate across platforms or scale across jurisdictions. Regulatory divergence, inconsistent data standards and unresolved governance challenges continue to constrain interoperability, limiting scale and system-wide impact. Infrastructure and connectivity gaps further limit adoption in lower-resource settings. As a result, innovation has advanced without corresponding transformation at the system level and health systems have not been able to capture the productivity gains or cost efficiencies that these technologies could support at scale.
McKinsey Global Institute estimates that digital health interventions – including remote monitoring, AI and automation – could generate between $1.5 and $3 trillion in annual efficiency savings globally by 2030.
A new paradigm of care is emerging that is worthy of greater attention. “Virtual health” is often described as care delivered at a distance; however, this premise mistakes geography for substance. It is a technology-enabled layer that dissolves the primacy of place, allowing care to be organized around need rather than location. As it embeds within integrated systems, the distinction between remote and on-site becomes increasingly irrelevant, what follows is not an extension of traditional models, but rather an evolution to new models that centre on people. In this sense, virtual health is not a parallel system, but an enabler of more resilient, adaptive and inclusive health systems.
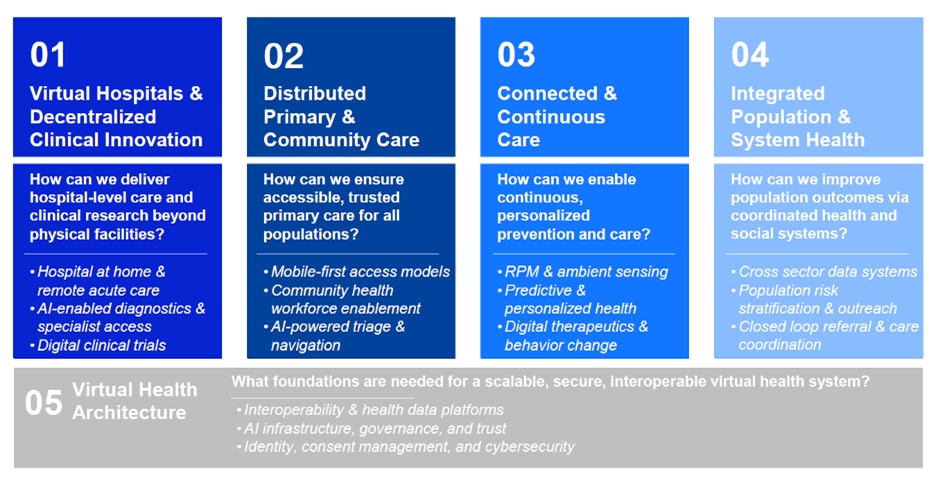
Four economies building momentum in virtual health
Early implementations are already demonstrating impact at scale across major health systems. Here are four case studies.
Saudi Arabia’s Seha Virtual Hospital hosts one of the world's largest national virtual care systems. It links 224 hospitals and facilitates over 16 million virtual appointments, spanning emergency triage, specialist referrals and chronic disease management. Alongside it, the Sehhaty digital health platform provides millions of users with a single digital entry point for consultations, prescriptions, referrals and health information.
In the US, where cost pressures are among the highest globally, virtual health has become a critical tool for addressing rural access gaps and improving care coordination. Telehealth expansion – accelerated during the COVID-19 pandemic – has enabled patients in remote areas to access primary and specialist care, while integrated virtual care models are increasingly used to manage chronic conditions, reduce hospital readmissions and support continuity across fragmented systems.
In China, rapid advances in AI-enabled healthcare and “internet hospitals” are reshaping service delivery. Large platforms integrate virtual consultations, AI-assisted diagnostics, e-prescriptions and home delivery of medicines, enabling high-volume, technology-enabled care. AI is also being deployed to support clinical decision-making and population health management at scale.
In India, the government has scaled telemedicine nationally through the eSanjeevani platform, which has enabled hundreds of millions of consultations by connecting patients in rural and underserved areas with doctors across the country. Private providers have complemented this system; for instance Apollo Hospitals has built one of South Asia’s largest multi-specialty telemedicine networks, reaching more than 20 million individuals through over 350,000 touch points and expanding access to specialist care across geographies.
Across these systems, virtual health is anchored within national or system-wide strategies and virtual services are thoughtfully integrated into existing care models, rather than in parallel. Despite this progress, several challenges –including limited interoperability, fragmented regulation, misaligned incentives, uneven workforce and patient adoption, and persistent gaps in digital access – continue to limit virtual health’s impact, reinforcing the need for more coordinated approache to implementation.
Seizing this moment for virtual health
Today, several enabling conditions have converged. Advances in artificial intelligence, cloud infrastructure and connected devices have dramatically expanded technical capabilities. Post-pandemic normalization of remote care, mounting fiscal pressures and rising public expectations have created greater policy openness to change. Together, these conditions create a window for structural reform. However, without coordinated global leadership, progress will remain fragmented.
The institutional landscape for global health cooperation is becoming more diffuse, with greater emphasis on regional and bilateral approaches. Without global alignment, progress will continue unevenly across countries and systems, limiting the overall impact.
The priorities shaping this year's 79th World Health Assembly and the World Economic Forum’s Annual Health Roundtable reflect this urgency. From harmonizing governance and standards for digital health AI, to addressing the global health workforce crisis, advancing implementation of the Pandemic Agreement, restoring progress toward universal health coverage and building systems that are resilient to climate-related disruption – each of these requires delivery models that can operate beyond the constraints of physical infrastructure and adapt to changing conditions. Virtual health offers a set of capabilities that directly support these objectives. It enables continuous management of chronic conditions, expanded access for underserved populations, and more proactive, patient-centred systems.
A critical window is now open. The convergence of technological readiness, policy momentum and urgency presents a unique opportunity to shape the future of care delivery. Realizing this opportunity will depend not only on innovation, but on sustained collaboration across the public and private sectors and across borders.
Don't miss any update on this topic
Create a free account and access your personalized content collection with our latest publications and analyses.
License and Republishing
World Economic Forum articles may be republished in accordance with the Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International Public License, and in accordance with our Terms of Use.
The views expressed in this article are those of the author alone and not the World Economic Forum.
Stay up to date:
Virtual and Augmented Reality
Forum Stories newsletter
Bringing you weekly curated insights and analysis on the global issues that matter.
More on Health and Healthcare SystemsSee all
David E. Bloom, Monica H. Carney, Joseph S. Knee and Julian C. Palladino
May 15, 2026