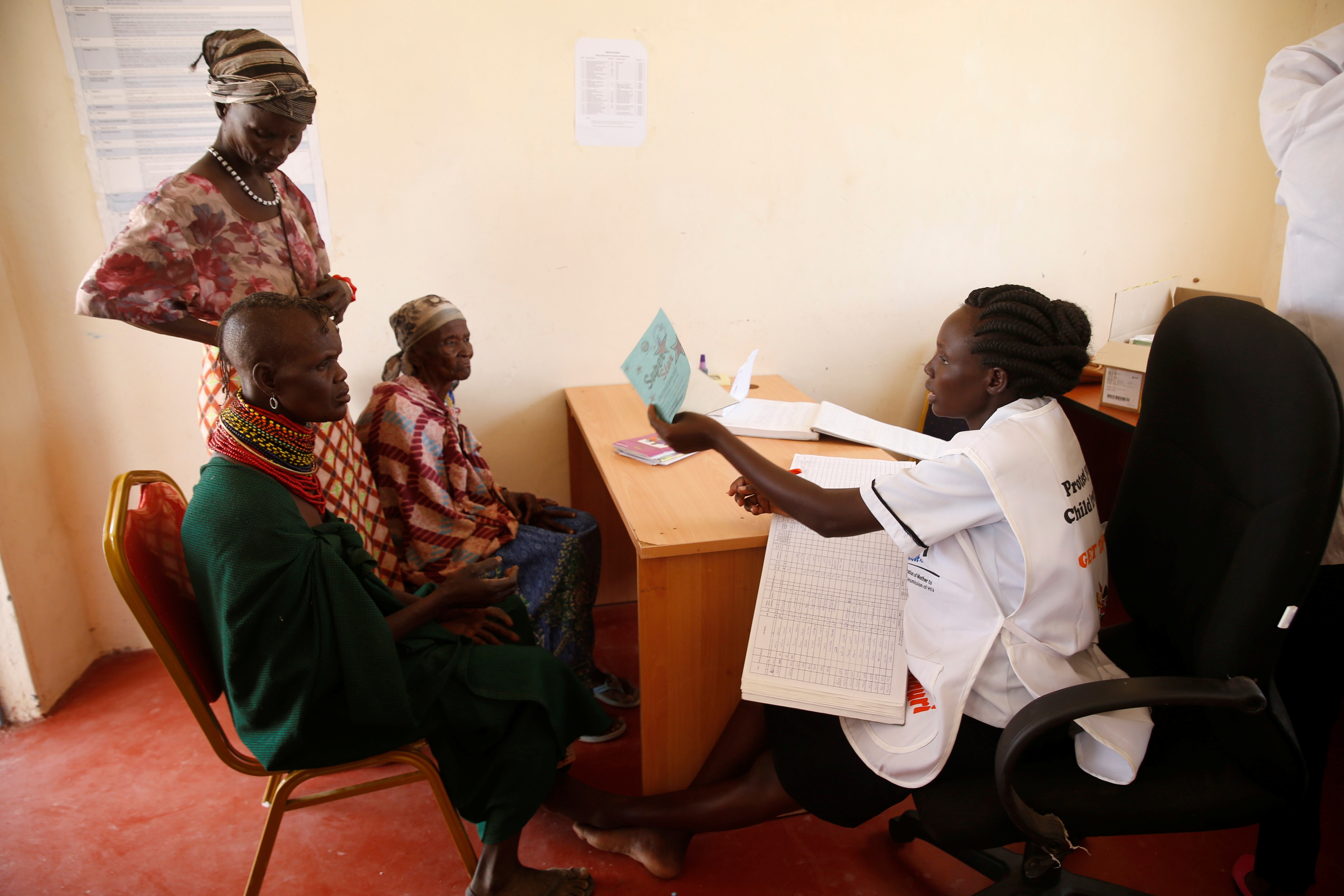
How greater spending on preventive health can promote economic growth
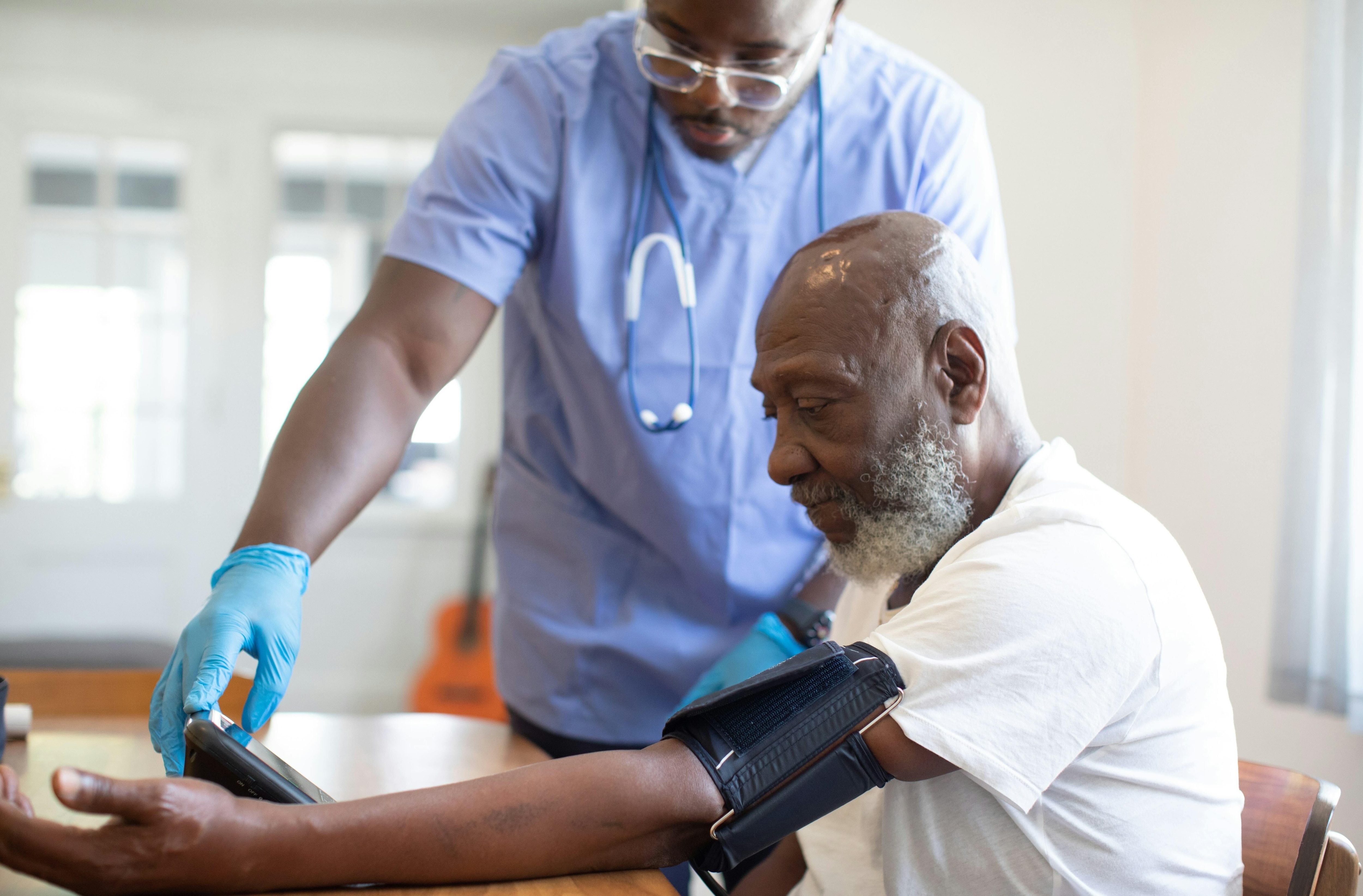
In Europe, governments must acknowledge the investment value of spending on preventive health Image: Nappystudio/Unsplash
David E. Bloom
Clarence James Gamble Professor of Economics and Demography, Harvard TH Chan School of Public Health (HSPH)- EU Member States are facing considerable budgetary pressure from multiple sources, such as increased defence spending targets and population ageing.
- These pressures are driving public expenditures upward, magnifying the challenge Member States feel as they seek to control spending to comply with the Stability and Growth Pact’s debt and deficit limits.
- Because of its substantial investment value, spending on preventive health, especially immunisation, may be a potent tool for addressing budgetary pressures in the coming years.
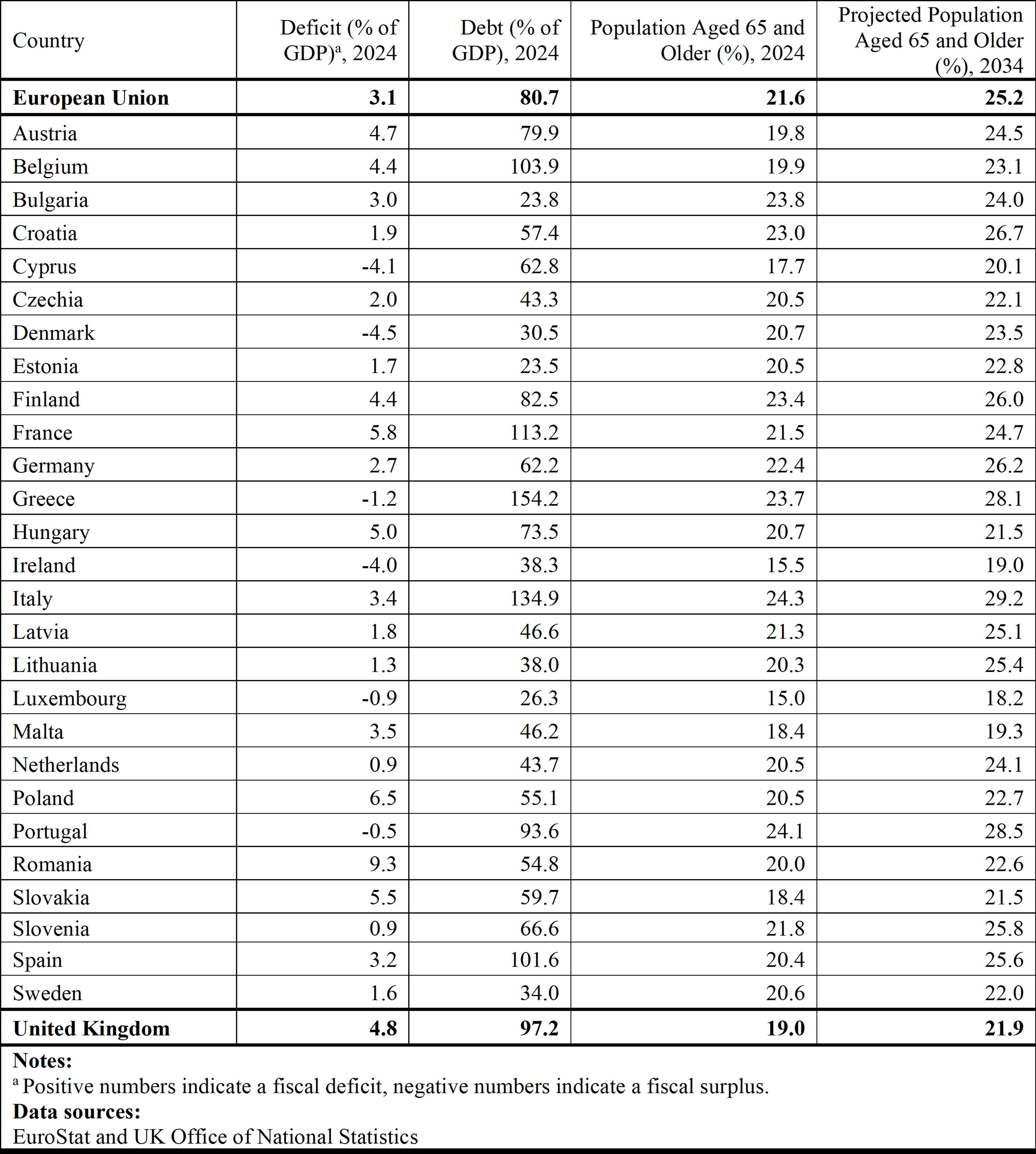
Member States of the EU face considerable budgetary pressure. In 2025, NATO allies (which include most EU Member States) agreed to increase defence spending from a target of 2% to 5% of GDP by 2035. With over one quarter of the EU population projected to be aged 65 years or older by 2034 (Table 1), Member States are also anticipating growing budgetary commitments for pensions and for health and other long-term care expenditures.
In addition, grants and loans to Member States through the temporary NextGenerationEU economic recovery instrument, created in response to the COVID-19 pandemic, will be phased out by the end of this year, with loan repayment beginning in 2028.
Table 1: Characteristics of EU Member States and the United Kingdom:
These pressures are driving public expenditures upward, magnifying the challenge Member States feel as they seek to control spending in an effort to comply with the Stability and Growth Pact’s (SGP) requirements to limit annual public deficits to 3% of GDP and public debt to 60% of GDP. Adherence to these limits is intended to keep a lid on inflation and interest rates and to promote a stable economic growth trajectory among Member States. The Great Recession and the associated European debt crisis, however, pushed many Member States out of compliance for much of the 2010s.
More recently, enforcement of the deficit and debt limits was suspended in 2020 in response to the economic pressures of the COVID-19 pandemic, with an elevated number of Member States out of compliance when enforcement resumed in 2024 (Table 1). Also in 2024, a new economic governance framework was introduced to flexibly facilitate a return to compliance with the SGP limits and to promote sustainable and inclusive economic growth.
Under this framework, each Member State was required to submit a medium-term fiscal-structural plan outlining (net) expenditure paths, structural reforms, and planned investments to ensure compliance by the end of a four-year adjustment period. The adjustment period can be extended to seven years if Member States demonstrate a commitment to structural reforms and investments aimed at boosting productivity in the medium- and long-run and at addressing core EU priorities: defence, digital transition, green transition, and social and economic resilience.
Population health as a driver of economic growth
Resilience is strengthened by investments in human capital, such as education and workforce skills. In recent years, theory, evidence, and common sense have also identified population health as a major form of human capital with significant implications for macroeconomic performance. This shift in thinking reflects the fact that healthy adults tend to work more, be more productive, contribute more to tax receipts, and create more value in non-market settings; healthy children receive more schooling and learn more, and tend to have higher adult earnings; and healthy populations save and invest more, as well as attract more direct foreign investment and growth-enhancing technology transfers and trade.
The outsized investment value of preventive health spending
The case for treating spending on health as an investment is particularly strong for spending on preventive health, which includes both access and innovation with respect to mass immunisation, screening, and early detection programmes; environmental and community health measures; workplace and school-based efforts aimed at disease prevention and health literacy; and preventive medications.
A wide range of such preventive health interventions, including smoking cessation, cancer screenings, statin therapy, and HIV pre-exposure prophylaxis in high-risk populations, has been shown to be cost-effective in Europe. But perhaps the strongest evidence that spending on preventive health has investment value comes from studies of immunisation programmes.
A recent publication found that the returns on adult immunisation around the world are estimated to be as high as 19 times the cost. In Europe, vaccines such as those to prevent influenza and pneumococcal disease have been shown to be cost-effective or cost-saving across all life stages. In addition, the HPV vaccine offers a high return on investment, and multiple paediatric immunisation programmes in Europe have been found to have high benefit-cost ratios, with up to €8.5 in value created for every €1 spent on those programmes. While such programmes are valued over patients’ lifetimes, the dominant share of the benefits is reaped in their first ten years in operation.
Preventive health spending, particularly on immunisation, is likely to soon result in even higher value-for-money. This expected enhancement has three drivers. The first driver has to do with scientific advances associated with AI. When applied to complex biological datasets, AI can accelerate the process of vaccine development.
The COVID-19 pandemic highlighted the value of rapid vaccine development to countries’ population health and their economies. The second driver reflects vaccines’ great potential to mitigate the health and economic losses expected to accompany the further growth of antimicrobial resistance. The third driver is population ageing. Spending on preventive health elevates market and non-market productivity and promotes longer working lives, increasing income and tax receipts and reducing the burden of age-related health and social care costs.
The growing value of preventive health interventions will only be realized if governments are willing to spend on their continued development and delivery, which includes redressing the issue of low vaccine coverage rates (Table 2). Currently, however, spending on preventive health represents only a small share of total health spending across the EU (typically around 3%; see Figure 1). Increasing this spending need not be a burden with respect to compliance with the SGP’s limits given its investment properties, which some countries are already recognising.
Table 2: Selected Annual Vaccination Coverage Ratesa (2024) for EU Member States and for the United Kingdom:
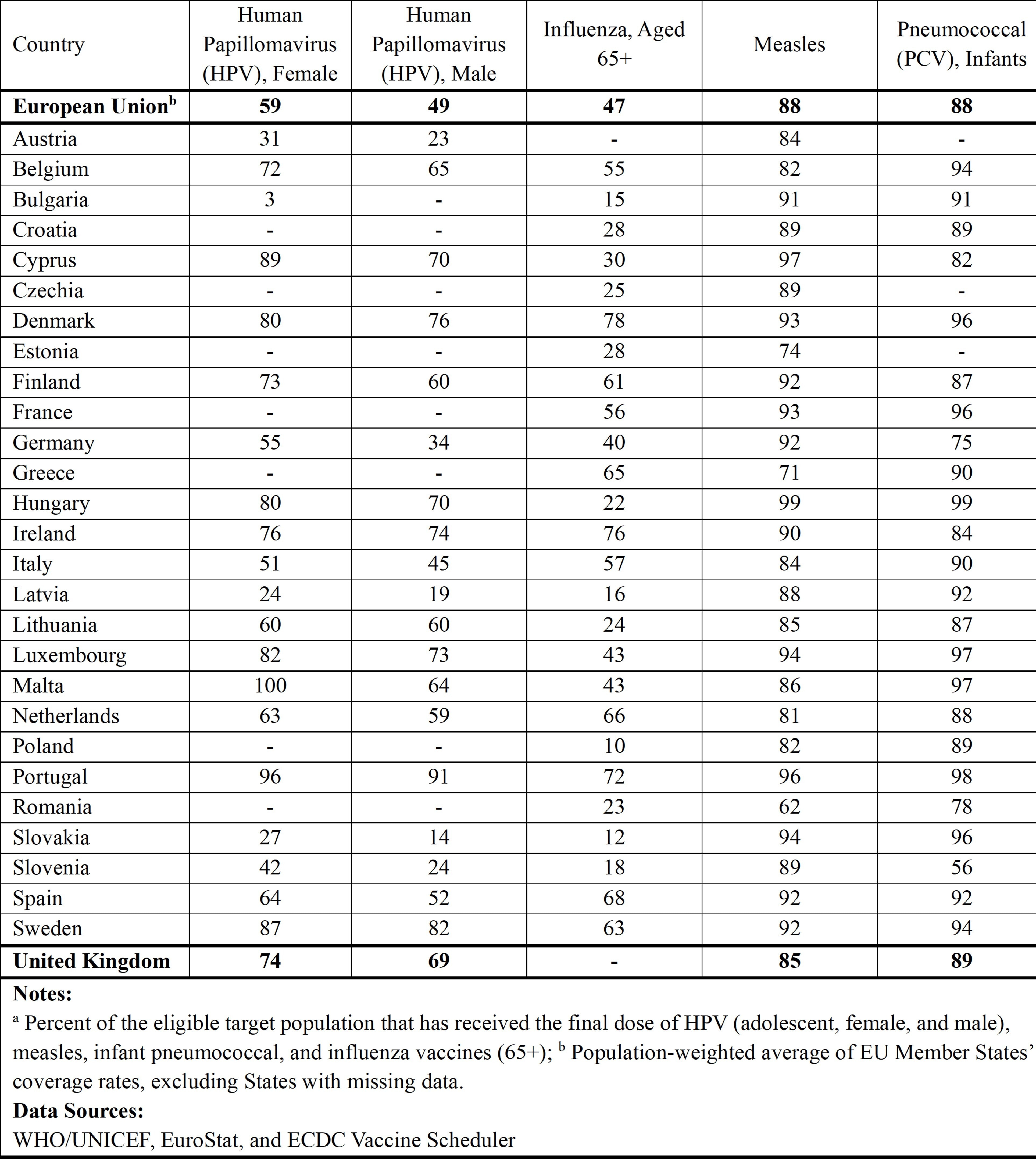
Figure 1: Government Preventive Health Spending in the EU and in the UK:
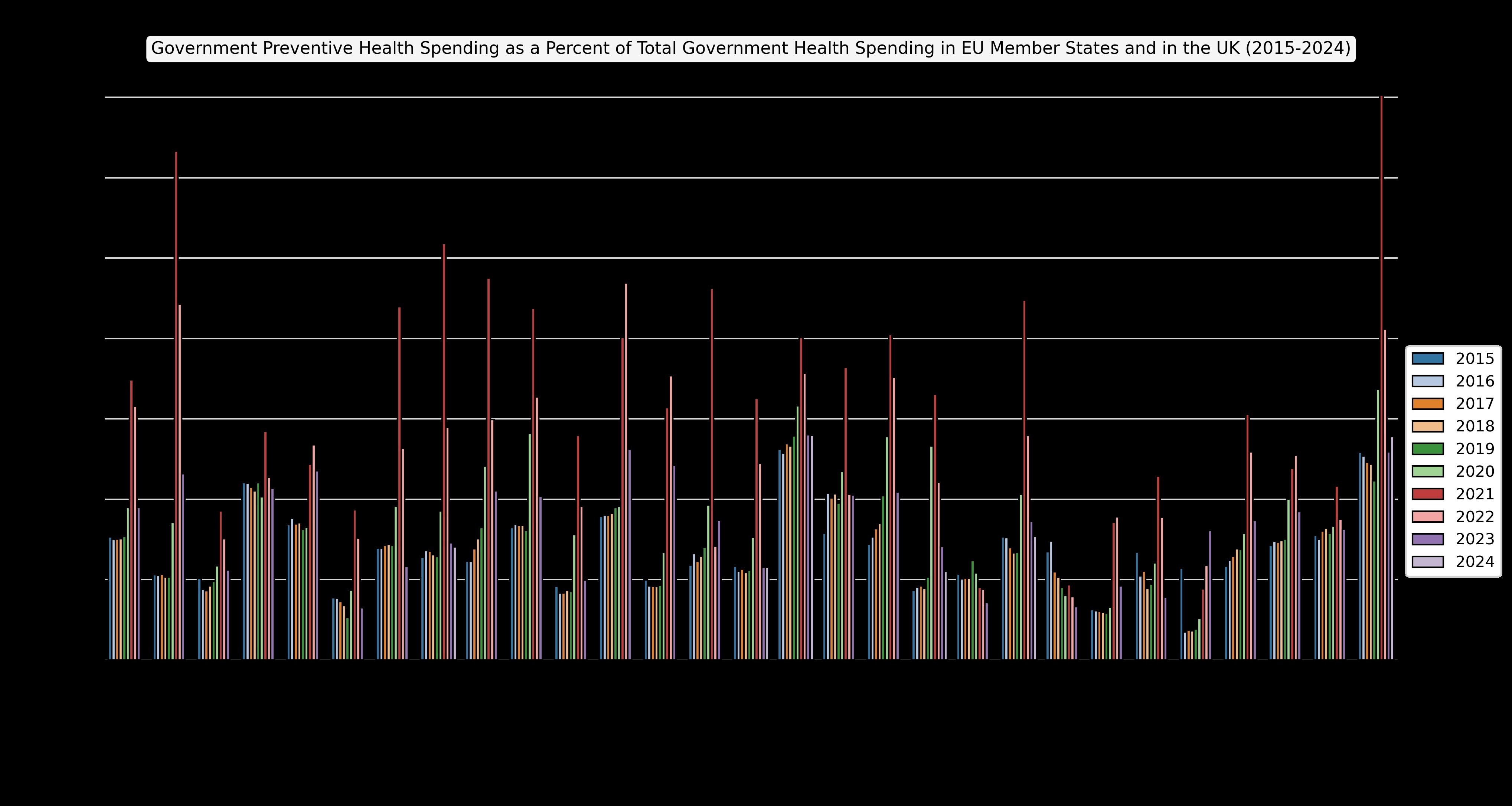
Conclusion
EU Member States face significant economic and demographic headwinds, adding pressure to many already swollen public spending budgets. But spending on preventive health can be a potent instrument for addressing deficit, debt, and economic growth challenges. The flexibility associated with the reforms of the new economic governance framework gives spending on preventive health interventions time to produce meaningful economic returns as Member States work to satisfy their SGP compliance obligations. Attention to this observation will afford leaders of the EU Member States a win-win opportunity: promoting both the health and economic wellbeing of their populations.
Don't miss any update on this topic
Create a free account and access your personalized content collection with our latest publications and analyses.
License and Republishing
World Economic Forum articles may be republished in accordance with the Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International Public License, and in accordance with our Terms of Use.
The views expressed in this article are those of the author alone and not the World Economic Forum.
Stay up to date:
Economic Growth
Forum Stories newsletter
Bringing you weekly curated insights and analysis on the global issues that matter.
More on Health and Healthcare SystemsSee all
Kaitlin Christenson, Ramiz Khan and Anna Bode
May 15, 2026